Adult Primary Liver Cancer Treatment (PDQ®): Treatment – Patient Information [NCI]
This information is produced and provided by the National Cancer Institute (NCI). The information in this topic may have changed since it was written. For the most current information, contact the National Cancer Institute via the Internet web site at http://cancer.gov or call 1-800-4-CANCER.
General Information About Adult Primary Liver Cancer
Adult primary liver cancer is a disease in which malignant (cancer) cells form in the tissues of the liver.
The liver is one of the largest organs in the body. It has two lobes and fills the upper right side of the abdomen inside the rib cage. Three of the many important functions of the liver are:
- To filter harmful substances from the blood so they can be passed from the body in stools and urine.
- To make bile to help digest fat that comes from food.
- To store glycogen (sugar), which the body uses for energy.
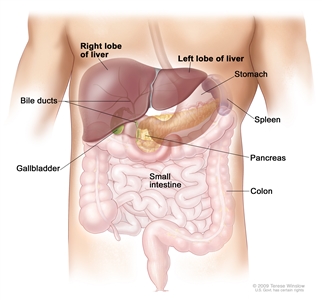
Anatomy of the liver. The liver is in the upper abdomen near the stomach, intestines, gallbladder, and pancreas. The liver has a right lobe and a left lobe. Each lobe is divided into two sections (not shown).
There are two types of adult primary liver cancer.
The two types of adult primary liver cancer are:
- Hepatocellular carcinoma.
- Cholangiocarcinoma (bile duct cancer). (See the PDQ summary on Bile Duct Cancer (Cholangiocarcinoma) Treatment for more information.)
The most common type of adult primary liver cancer is hepatocellular carcinoma. This type of liver cancer is the third leading cause of cancer-related deaths worldwide.
This summary is about the treatment of primary liver cancer (cancer that begins in the liver). Treatment of cancer that begins in other parts of the body and spreads to the liver is not covered in this summary.
Primary liver cancer can occur in both adults and children. However, treatment for children is different than treatment for adults. (See the PDQ summary on Childhood Liver Cancer Treatment for more information.)
Having hepatitis or cirrhosis can affect the risk of adult primary liver cancer.
Anything that increases your chance of getting a disease is called a risk factor. Having a risk factor does not mean that you will get cancer; not having risk factors doesn’t mean that you will not get cancer. Talk to your doctor if you think you may be at risk for liver cancer.
Risk factors for liver cancer include the following:
- Having hepatitis B or hepatitis C infection. Having both hepatitis B and hepatitis C increases the risk even more.
- Having cirrhosis.
- Heavy alcohol use. Heavy alcohol use and having hepatitis B infection increases the risk even more.
- Eating foods tainted with aflatoxin (poison from a fungus that can grow on foods, such as grains and nuts, that have not been stored properly).
- Having nonalcoholic steatohepatitis (NASH), a condition in which fat builds up in the liver and may progress to inflammation of the liver and liver cell damage.
- Using tobacco, such as cigarette smoking.
- Having certain inherited or rare disorders that damage the liver, including the following:
- Hereditary hemochromatosis, an inherited disorder in which the body stores more iron than it needs. The extra iron is mostly stored in the liver, heart, pancreas, skin, and joints.
- Alpha-1 antitrypsin deficiency, an inherited disorder that can cause liver and lung disease.
- Glycogen storage disease, an inherited disorder in which there are problems with how a form of glucose (sugar) called glycogen is stored and used in the body.
- Porphyria cutanea tarda, a rare disorder that affects the skin and causes painful blisters on parts of the body that are exposed to the sun, such as the hands, arms, and face. Liver problems can also occur.
- Wilson disease, a rare inherited disorder in which the body stores more copper than it needs. The extra copper is stored in the liver, brain, eyes, and other organs.
Older age is the main risk factor for most cancers. The chance of getting cancer increases as you get older.
Signs and symptoms of adult primary liver cancer include a lump or pain on the right side.
These and other signs and symptoms may be caused by adult primary liver cancer or by other conditions. Check with your doctor if you have any of the following:
- A hard lump on the right side just below the rib cage.
- Discomfort in the upper abdomen on the right side.
- A swollen abdomen.
- Pain near the right shoulder blade or in the back.
- Jaundice (yellowing of the skin and whites of the eyes).
- Easy bruising or bleeding.
- Unusual tiredness or weakness.
- Nausea and vomiting.
- Loss of appetite or feelings of fullness after eating a small meal.
- Weight loss for no known reason.
- Pale, chalky bowel movements and dark urine.
- Fever.
Tests that examine the liver and the blood are used to detect (find) and diagnose adult primary liver cancer.
The following tests and procedures may be used:
- Physical exam and history: An exam of the body to check general signs of health, including checking for signs of disease, such as lumps or anything else that seems unusual. A history of the patient’s health habits and past illnesses and treatments will also be taken.
- Serum tumor marker test: A procedure in which a sample of blood is examined to measure the amounts of certain substances released into the blood by organs, tissues, or tumor cells in the body. Certain substances are linked to specific types of cancer when found in increased levels in the blood. These are called tumor markers. An increased level of alpha-fetoprotein (AFP) in the blood may be a sign of liver cancer. Other cancers and certain noncancerous conditions, including cirrhosis and hepatitis, may also increase AFP levels. Sometimes the AFP level is normal even when there is liver cancer.
- Liver function tests: A procedure in which a blood sample is checked to measure the amounts of certain substances released into the blood by the liver. A higher than normal amount of a substance can be a sign of liver cancer.
- CT scan (CAT scan): A procedure that makes a series of detailed pictures of areas inside the body, such as the abdomen, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography. Images may be taken at three different times after the dye is injected, to get the best picture of abnormal areas in the liver. This is called triple-phase CT. A spiral or helical CT scan makes a series of very detailed pictures of areas inside the body using an x-ray machine that scans the body in a spiral path.
- MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body, such as the liver. This procedure is also called nuclear magnetic resonance imaging (NMRI). To create detailed pictures of blood vessels in and near the liver, dye is injected into a vein. This procedure is called MRA (magnetic resonance angiography). Images may be taken at three different times after the dye is injected, to get the best picture of abnormal areas in the liver. This is called triple-phase MRI.
- Ultrasound exam: A procedure in which high-energy sound waves (ultrasound) are bounced off internal tissues or organs and make echoes. The echoes form a picture of body tissues called a sonogram. The picture can be printed to be looked at later.
- Biopsy: The removal of cells or tissues so they can be viewed under a microscope by a pathologist to check for signs of cancer. Procedures used to collect the sample of cells or tissues include the following:
- Fine-needle aspiration biopsy: The removal of cells, tissue or fluid using a thin needle.
- Core needle biopsy: The removal of cells or tissue using a slightly wider needle.
- Laparoscopy: A surgical procedure to look at the organs inside the abdomen to check for signs of disease. Small incisions (cuts) are made in the wall of the abdomen and a laparoscope (a thin, lighted tube) is inserted into one of the incisions. Another instrument is inserted through the same or another incision to remove the tissue samples.
A biopsy is not always needed to diagnose adult primary liver cancer.
Certain factors affect prognosis (chance of recovery) and treatment options.
The prognosis (chance of recovery) and treatment options depend on the following:
- The stage of the cancer (the size of the tumor, whether it affects part or all of the liver, or has spread to other places in the body).
- How well the liver is working.
- The patient’s general health, including whether there is cirrhosis of the liver.
Stages of Adult Primary Liver Cancer
After adult primary liver cancer has been diagnosed, tests are done to find out if cancer cells have spread within the liver or to other parts of the body.
The process used to find out if cancer has spread within the liver or to other parts of the body is called staging. The information gathered from the staging process determines the stage of the disease. It is important to know the stage in order to plan treatment. The following tests and procedures may be used in the staging process:
- CT scan (CAT scan): A procedure that makes a series of detailed pictures of areas inside the body, such as the chest, abdomen, and pelvis, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
- MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body. This procedure is also called nuclear magnetic resonance imaging (NMRI).
- PET scan (positron emission tomography scan): A procedure to find malignant tumor cells in the body. A small amount of radioactive glucose (sugar) is injected into a vein. The PET scanner rotates around the body and makes a picture of where glucose is being used in the body. Malignant tumor cells show up brighter in the picture because they are more active and take up more glucose than normal cells do.
There are three ways that cancer spreads in the body.
Cancer can spread through tissue, the lymph system, and the blood:
- Tissue. The cancer spreads from where it began by growing into nearby areas.
- Lymph system. The cancer spreads from where it began by getting into the lymph system. The cancer travels through the lymph vessels to other parts of the body.
- Blood. The cancer spreads from where it began by getting into the blood. The cancer travels through the blood vessels to other parts of the body.
Cancer may spread from where it began to other parts of the body.
When cancer spreads to another part of the body, it is called metastasis. Cancer cells break away from where they began (the primary tumor) and travel through the lymph system or blood.
- Lymph system. The cancer gets into the lymph system, travels through the lymph vessels, and forms a tumor (metastatic tumor) in another part of the body.
- Blood. The cancer gets into the blood, travels through the blood vessels, and forms a tumor (metastatic tumor) in another part of the body.
The metastatic tumor is the same type of cancer as the primary tumor. For example, if primary liver cancer spreads to the lung, the cancer cells in the lung are actually liver cancer cells. The disease is metastatic liver cancer, not lung cancer.
The Barcelona Clinic Liver Cancer Staging System may be used to stage adult primary liver cancer.
There are several staging systems for liver cancer. The Barcelona Clinic Liver Cancer (BCLC) Staging System is widely used and is described below. This system is used to predict the patient’s chance of recovery and to plan treatment, based on the following:
- Whether the cancer has spread within the liver or to other parts of the body.
- How well the liver is working.
- The general health and wellness of the patient.
- The symptoms caused by the cancer.
The BCLC staging system has five stages:
- Stage 0: Very early
- Stage A: Early
- Stage B: Intermediate
- Stage C: Advanced
- Stage D: End-stage
The following groups are used to plan treatment.
BCLC stages 0, A, and B
Treatment to cure the cancer is given for BCLC stages 0, A, and B.
BCLC stages C and D
Treatment to relieve the symptoms caused by liver cancer and improve the patient’s quality of life is given for BCLC stages C and D. Treatments are not likely to cure the cancer.
Recurrent Adult Primary Liver Cancer
Recurrent adult primary liver cancer is cancer that has recurred (come back) after it has been treated. The cancer may come back in the liver or in other parts of the body.
Treatment Option Overview
There are different types of treatment for patients with adult primary liver cancer.
Different types of treatments are available for patients with adult primary liver cancer. Some treatments are standard (the currently used treatment), and some are being tested in clinical trials. A treatment clinical trial is a research study meant to help improve current treatments or obtain information on new treatments for patients with cancer. When clinical trials show that a new treatment is better than the standard treatment, the new treatment may become the standard treatment. Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Patients with liver cancer are treated by a team of specialists who are experts in treating liver cancer.
The patient’s treatment will be overseen by a medical oncologist, a doctor who specializes in treating people with cancer. The medical oncologist may refer the patient to other health professionals who have special training in treating patients with liver cancer. These may include the following specialists:
- Hepatologist (specialist in liver disease).
- Surgical oncologist.
- Transplant surgeon.
- Radiation oncologist.
- Interventional radiologist (a specialist who diagnoses and treats diseases using imaging and the smallest incisions possible).
- Pathologist.
Eight types of standard treatment are used:
Surveillance
Surveillance for lesions smaller than 1 centimeter found during screening. Follow-up every three months is common.
Surgery
A partial hepatectomy (surgery to remove the part of the liver where cancer is found) may be done. A wedge of tissue, an entire lobe, or a larger part of the liver, along with some of the healthy tissue around it is removed. The remaining liver tissue takes over the functions of the liver and may regrow.
Liver transplant
In a liver transplant, the entire liver is removed and replaced with a healthy donated liver. A liver transplant may be done when the disease is in the liver only and a donated liver can be found. If the patient has to wait for a donated liver, other treatment is given as needed.
Ablation therapy
Ablation therapy removes or destroys tissue. Different types of ablation therapy are used for liver cancer:
- Radiofrequency ablation: The use of special needles that are inserted directly through the skin or through an incision in the abdomen to reach the tumor. High-energy radio waves heat the needles and tumor which kills cancer cells.
- Microwave therapy: A type of treatment in which the tumor is exposed to high temperatures created by microwaves. This can damage and kill cancer cells or make them more sensitive to the effects of radiation and certain anticancer drugs.
- Percutaneous ethanol injection: A cancer treatment in which a small needle is used to inject ethanol (pure alcohol) directly into a tumor to kill cancer cells. Several treatments may be needed. Usually local anesthesia is used, but if the patient has many tumors in the liver, general anesthesia may be used.
- Cryoablation: A treatment that uses an instrument to freeze and destroy cancer cells. This type of treatment is also called cryotherapy and cryosurgery. The doctor may use ultrasound to guide the instrument.
- Electroporation therapy: A treatment that sends electrical pulses through an electrode placed in a tumor to kill cancer cells. Electroporation therapy is being studied in clinical trials.
Embolization therapy
Embolization therapy is the use of substances to block or decrease the flow of blood through the hepatic artery to the tumor. When the tumor does not get the oxygen and nutrients it needs, it will not continue to grow. Embolization therapy is used for patients who cannot have surgery to remove the tumor or ablation therapy and whose tumor has not spread outside the liver.
The liver receives blood from the hepatic portal vein and the hepatic artery. Blood that comes into the liver from the hepatic portal vein usually goes to the healthy liver tissue. Blood that comes from the hepatic artery usually goes to the tumor. When the hepatic artery is blocked during embolization therapy, the healthy liver tissue continues to receive blood from the hepatic portal vein.
There are two main types of embolization therapy:
- Transarterial embolization (TAE): A small incision (cut) is made in the inner thigh and a catheter (thin, flexible tube) is inserted and threaded up into the hepatic artery. Once the catheter is in place, a substance that blocks the hepatic artery and stops blood flow to the tumor is injected.
- Transarterial chemoembolization (TACE): This procedure is like TAE except an anticancer drug is also given. The procedure can be done by attaching the anticancer drug to small beads that are injected into the hepatic artery or by injecting the anticancer drug through the catheter into the hepatic artery and then injecting the substance to block the hepatic artery. Most of the anticancer drug is trapped near the tumor and only a small amount of the drug reaches other parts of the body. This type of treatment is also called chemoembolization.
Targeted therapy
Targeted therapy is a treatment that uses drugs or other substances to identify and attack specific cancer cells without harming normal cells. Tyrosine kinase inhibitors are a type of targeted therapy used in the treatment of adult primary liver cancer.
Tyrosine kinase inhibitors are small-molecule drugs that go through the cell membrane and work inside cancer cells to block signals that cancer cells need to grow and divide. Some tyrosine kinase inhibitors also have angiogenesis inhibitor effects. Sorafenib, lenvatinib, and regorafenib are types of tyrosine kinase inhibitors.
See Drugs Approved for Liver Cancer for more information.
Immunotherapy
Immunotherapy is a treatment that uses the patient’s immune system to fight cancer. Substances made by the body or made in a laboratory are used to boost, direct, or restore the body’s natural defenses against cancer. This type of cancer treatment is also called biotherapy or biologic therapy.
Immune checkpoint inhibitor therapy is a type of immunotherapy.
- Immune checkpoint inhibitor therapy: PD-1 is a protein on the surface of T cells that helps keep the body’s immune responses in check. When PD-1 attaches to another protein called PDL-1 on a cancer cell, it stops the T cell from killing the cancer cell. PD-1 inhibitors attach to PDL-1 and allow the T cells to kill cancer cells. Nivolumab is a type of immune checkpoint inhibitor.
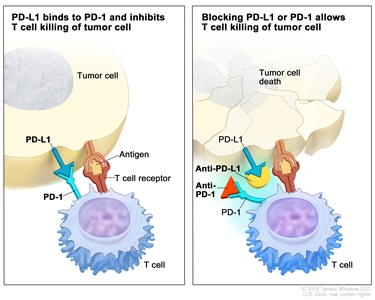
Immune checkpoint inhibitor. Checkpoint proteins, such as PD-L1 on tumor cells and PD-1 on T cells, help keep immune responses in check. The binding of PD-L1 to PD-1 keeps T cells from killing tumor cells in the body (left panel). Blocking the binding of PD-L1 to PD-1 with an immune checkpoint inhibitor (anti-PD-L1 or anti-PD-1) allows the T cells to kill tumor cells (right panel).
See Drugs Approved for Liver Cancer for more information.
Radiation therapy
Radiation therapy is a cancer treatment that uses high-energy x-rays or other types of radiation to kill cancer cells or keep them from growing. There are two types of radiation therapy:
- External radiation therapy uses a machine outside the body to send radiation toward the cancer. Certain ways of giving radiation therapy can help keep radiation from damaging nearby healthy tissue. These types of external radiation therapy include the following:
- Conformal radiation therapy: Conformal radiation therapy is a type of external radiation therapy that uses a computer to make a 3-dimensional (3-D) picture of the tumor and shapes the radiation beams to fit the tumor. This allows a high dose of radiation to reach the tumor and causes less damage to nearby healthy tissue.
- Stereotactic body radiation therapy: Stereotactic body radiation therapy is a type of external radiation therapy. Special equipment is used to place the patient in the same position for each radiation treatment. Once a day for several days, a radiation machine aims a larger than usual dose of radiation directly at the tumor. By having the patient in the same position for each treatment, there is less damage to nearby healthy tissue. This procedure is also called stereotactic external-beam radiation therapy and stereotaxic radiation therapy.
- Proton beam radiation therapy: Proton-beam therapy is a type of high-energy, external radiation therapy. A radiation therapy machine aims streams of protons (tiny, invisible, positively-charged particles) at the cancer cells to kill them. This type of treatment causes less damage to nearby healthy tissue.
- Internal radiation therapy uses a radioactive substance sealed in needles, seeds, wires, or catheters that are placed directly into or near the cancer.
The way the radiation therapy is given depends on the type and stage of the cancer being treated. External radiation therapy is used to treat adult primary liver cancer.
New types of treatment are being tested in clinical trials.
Information about clinical trials is available from the NCI website.
Treatment for adult primary liver cancer may cause side effects.
For information about side effects caused by treatment for cancer, see our Side Effects page.
Patients may want to think about taking part in a clinical trial.
For some patients, taking part in a clinical trial may be the best treatment choice. Clinical trials are part of the cancer research process. Clinical trials are done to find out if new cancer treatments are safe and effective or better than the standard treatment.
Many of today’s standard treatments for cancer are based on earlier clinical trials. Patients who take part in a clinical trial may receive the standard treatment or be among the first to receive a new treatment.
Patients who take part in clinical trials also help improve the way cancer will be treated in the future. Even when clinical trials do not lead to effective new treatments, they often answer important questions and help move research forward.
Patients can enter clinical trials before, during, or after starting their cancer treatment.
Some clinical trials only include patients who have not yet received treatment. Other trials test treatments for patients whose cancer has not gotten better. There are also clinical trials that test new ways to stop cancer from recurring (coming back) or reduce the side effects of cancer treatment.
Clinical trials are taking place in many parts of the country. Information about clinical trials supported by NCI can be found on NCI’s clinical trials search webpage. Clinical trials supported by other organizations can be found on the ClinicalTrials.gov website.
Follow-up tests may be needed.
Some of the tests that were done to diagnose the cancer or to find out the stage of the cancer may be repeated. Some tests will be repeated in order to see how well the treatment is working. Decisions about whether to continue, change, or stop treatment may be based on the results of these tests.
Some of the tests will continue to be done from time to time after treatment has ended. The results of these tests can show if your condition has changed or if the cancer has recurred (come back). These tests are sometimes called follow-up tests or check-ups.
Treatment Options for Adult Primary Liver Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
Stages 0, A, and B Adult Primary Liver Cancer
Treatment of stages 0, A, and B adult primary liver cancer may include the following:
- Surveillance for lesions smaller than 1 centimeter.
- Partial hepatectomy.
- Total hepatectomy and liver transplant.
- Ablation of the tumor using one of the following methods:
- Radiofrequency ablation.
- Microwave therapy.
- Percutaneous ethanol injection.
- Cryoablation.
- A clinical trial of electroporation therapy.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Stages C and D Adult Primary Liver Cancer
Treatment of stages C and D adult primary liver cancer may include the following:
- Embolization therapy using one of the following methods:
- Transarterial embolization (TAE).
- Transarterial chemoembolization (TACE).
- Targeted therapy with a tyrosine kinase inhibitor.
- Immunotherapy.
- Radiation therapy.
- A clinical trial of targeted therapy after chemoembolization or combined with chemotherapy.
- A clinical trial of new targeted therapy drugs.
- A clinical trial of immunotherapy.
- A clinical trial of immunotherapy combined with targeted therapy.
- A clinical trial of stereotactic body radiation therapy or proton-beam radiation therapy.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Recurrent Adult Primary Liver Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment options for recurrent adult primary liver cancer may include the following:
- Total hepatectomy and liver transplant.
- Partial hepatectomy.
- Ablation
- Transarterial chemoembolization and targeted therapy with sorafenib, as palliative therapy to relieve symptoms and improve quality of life.
- A clinical trial of a new treatment.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
To Learn More About Adult Primary Liver Cancer
For more information from the National Cancer Institute about adult primary liver cancer, see the following:
- Liver and Bile Duct Cancer Home Page
- Liver (Hepatocellular) Cancer Prevention
- Liver (Hepatocellular) Cancer Screening
- Cryosurgery in Cancer Treatment
- Drugs Approved for Liver Cancer
- Targeted Cancer Therapies
For general cancer information and other resources from the National Cancer Institute, see the following:
- About Cancer
- Staging
- Chemotherapy and You: Support for People With Cancer
- Radiation Therapy and You: Support for People With Cancer
- Coping with Cancer
- Questions to Ask Your Doctor about Cancer
- For Survivors and Caregivers
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute’s (NCI’s) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government’s center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about the treatment of adult primary liver cancer. It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary (“Updated”) is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Adult Treatment Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become “standard.” Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI’s website. For more information, call the Cancer Information Service (CIS), NCI’s contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as “NCI’s PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary].”
The best way to cite this PDQ summary is:
PDQ® Adult Treatment Editorial Board. PDQ Adult Primary Liver Cancer Treatment. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/types/liver/patient/adult-liver-treatment-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389251]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website’s E-mail Us.
Last Revised: 2019-07-02
If you want to know more about cancer and how it is treated, or if you wish to know about clinical trials for your type of cancer, you can call the NCI’s Cancer Information Service at 1-800-422-6237, toll free. A trained information specialist can talk with you and answer your questions.
Topic Contents
- General Information About Adult Primary Liver Cancer
- Stages of Adult Primary Liver Cancer
- Recurrent Adult Primary Liver Cancer
- Treatment Option Overview
- Treatment Options for Adult Primary Liver Cancer
- Treatment of Recurrent Adult Primary Liver Cancer
- To Learn More About Adult Primary Liver Cancer
- About This PDQ Summary
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.

