Asthma in Teens and Adults
Topic Overview
Is this topic for you?
This topic provides information about asthma in teens and adults. If you are looking for information about asthma in children age 12 and younger, see the topic Asthma in Children.
What is asthma?
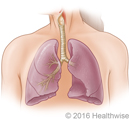
Asthma causes swelling and inflammation in the airways that lead to your lungs. When asthma flares up, the airways tighten and become narrower. This keeps the air from passing through easily and makes it hard for you to breathe. These flare-ups are also called asthma attacks or exacerbations (say “ig-zas-er-BAY-shuns”).
Asthma affects people in different ways. Some people have asthma attacks only during allergy season, or when they breathe in cold air, or when they exercise. Others have many bad attacks that send them to the doctor often.
Even if you have few asthma attacks, you still need to treat your asthma. The swelling and inflammation in your airways can lead to permanent changes in your airways and harm your lungs.
Many people with asthma live active, full lives. Although asthma is a lifelong disease, treatment can help control it and help you stay healthy.
What causes asthma?
Experts don’t know exactly what causes asthma. But there are some things we do know:
- Asthma runs in families.
- Asthma is much more common in people who have allergies, though not everyone with allergies gets asthma. And not everyone with asthma has allergies.
- Pollution may cause asthma or make it worse.
What are the symptoms?
Symptoms of asthma can be mild or severe. You may have mild attacks now and then, or you may have severe symptoms every day. Or you may have something in between. How often you have symptoms can also change. When you have asthma, you may:
- Wheeze, making a loud or soft whistling noise when you breathe in and out.
- Cough a lot.
- Feel tightness in your chest.
- Feel short of breath.
- Have trouble sleeping because of coughing or having a hard time breathing.
- Quickly get tired during exercise.
Your symptoms may be worse at night.
Severe asthma attacks can be life-threatening and need emergency treatment.
How is asthma diagnosed?
Along with doing a physical exam and asking about your health, your doctor may order lung function tests. These tests include:
- Spirometry. Doctors use this test to diagnose and keep track of asthma. It measures how quickly you can move air in and out of your lungs and how much air you move.
- Peak expiratory flow (PEF). This shows how much air you can breathe out when you try your hardest.
- An exercise or inhalation challenge. This test measures how your breathing is affected by exercise or after taking a medicine.
- A chest X-ray, to see if another disease is causing your symptoms.
- Allergy tests, if your doctor thinks your symptoms may be caused by allergies.
You will need routine checkups with your doctor to keep track of your asthma and decide on treatment.
How is it treated?
There are two parts to treating asthma, which are outlined in your asthma action plan. The goals are to:
- Control asthma over the long term. Your asthma action plan tells you which medicine to take. It also helps you track your symptoms and know how well the treatment is working. Many people take controller medicine—usually an inhaled corticosteroid—every day. Taking it every day helps to reduce the swelling of the airways and prevent attacks. Your doctor will show you how to use your inhaler correctly. This is very important so you get the right amount of medicine to help you breathe better.
- Treat asthma attacks when they occur. Your asthma action plan tells you what to do when you have an asthma attack. It helps you identify triggers that can cause your attacks. You use quick-relief medicine, such as albuterol, during an attack.
If you need to use the quick-relief inhaler more often than usual, talk to your doctor. This may be a sign that your asthma is not controlled and can cause problems.
Asthma attacks can be life-threatening, but you may be able to prevent them if you follow a plan. Your doctor can teach you the skills you need to use your asthma action plan.
How can you prevent asthma attacks?
You can prevent some asthma attacks by avoiding those things that cause them. These are called triggers. A trigger can be:
- Irritants in the air, such as cigarette smoke or other kinds of air pollution. Don’t smoke, and try to avoid being around others when they smoke.
- Things you are allergic to, such as pet dander, dust mites, cockroaches, or pollen. When you can, avoid those things you are allergic to. It may also help to take certain kinds of allergy medicine.
- Exercise. Ask your doctor about using a quick-relief inhaler before you exercise if this is a trigger for you.
- Other things like dry, cold air; an infection; or some medicines, such as aspirin and other nonsteroidal anti-inflammatory drugs (NSAIDs). Try not to exercise outside when it is cold and dry. Talk to your doctor about vaccines to prevent some infections. And ask about what medicines you should avoid.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
Cause
The cause of asthma isn’t known. Health experts believe that inherited, environmental, and immune system factors combine to cause inflammation of the airways. This can lead to asthma and asthma attacks.
Family history
Asthma may run in families (be inherited). If this is the case in your family, you may be more likely than other people to get long-lasting (chronic) inflammation in the airways.
Immune system
In some people, an allergic reaction causes asthma symptoms. An allergen makes the immune system cells release chemicals that cause inflammation.
Studies show that exposure to allergens such as dust mites, cockroaches, and animal dander may influence asthma’s development. Asthma is much more common in people who have allergies. But not all people who have allergies get asthma. And not all those who have asthma have allergies.
Environment
Environmental factors and today’s germ-conscious lifestyle may play a role in the development of asthma. Some experts believe that there are more cases of asthma because of pollution and less exposure to certain types of bacteria or infections.footnote 1 As a result, children’s immune systems may develop in a way that makes it more likely they will also get allergies and asthma.
Asthma in adults also can be related to exposure to substances at work. This is called occupational asthma.
Symptoms
Symptoms of asthma can be mild or severe. You may have no symptoms, severe symptoms every day, or something in between. How often you have symptoms can also change. Symptoms of asthma may include:
- Wheezing, which is a whistling noise of varying loudness that occurs when the airways of the lungs narrow.
- Coughing. This is the only symptom for some people.
- Chest tightness.
- Shortness of breath, which is rapid, shallow breathing, or difficulty breathing.
- Sleep disturbance because of coughing or having a hard time breathing.
- Tiring quickly during exercise.
An asthma attack occurs when your symptoms suddenly increase. Factors that can lead to an asthma attack or make it worse include:
- Having a cold or another type of respiratory illness, especially one caused by a virus, such as influenza.
- Exercising (exercise-induced asthma), especially if the air is cold and dry.
- Exposure to triggers, such as cigarette smoke, air pollution, dust mites, or animal dander.
- Being around chemicals or other substances at work (occupational asthma).
- Changes in hormones, such as during the start of a woman’s menstrual blood flow or pregnancy.
- Taking medicines, such as aspirin (aspirin-induced asthma) or nonsteroidal anti-inflammatory drugs.
Nighttime asthma
Many people have symptoms that become worse at night (nocturnal asthma), such as a cough and shortness of breath.
In general, waking at night because of shortness of breath or a cough is a sign of poorly controlled asthma.
What Happens
Asthma often begins during infancy or childhood, but it can start at any age. It may last throughout your life.
At times, the inflammation from asthma causes a narrowing of your airways and mucus production. This causes asthma symptoms such as shortness of breath.
Asthma attacks and what makes them worse
Your airways narrow when they overreact to certain substances. These are known as asthma triggers. What triggers asthma symptoms varies from person to person.
When asthma symptoms suddenly occur, it is called an asthma attack (also called a flare-up or exacerbation). Asthma attacks can occur rarely or frequently. They may be mild to severe.
Although some asthma attacks occur very suddenly, many become worse gradually over a period of several days. In general, you can take care of symptoms at home by following your asthma action plan. A severe attack may need emergency treatment and in rare cases can be fatal.
Asthma is classified as intermittent, mild persistent, moderate persistent, and severe persistent.
Effect on your long-term health
Asthma can raise your risk for complications from lung infections, such as acute bronchitis and pneumonia.
Even mild asthma may cause changes to the airway system. It may speed up and make worse the natural decrease in lung function that occurs as we age.
Some experts believe that asthma may raise your risk for chronic obstructive pulmonary disease (COPD).footnote 2
Asthma during pregnancy
Asthma can occur for the first time during pregnancy, or it may change during pregnancy.
When asthma is properly controlled, a woman can have a normal pregnancy with little or no increased risk to herself or the baby. But if the asthma isn’t well controlled, there are risks to the pregnant woman and the baby.
What Increases Your Risk
Many things can increase your risk for asthma. Some of these are not within your control. Others you can control.
The main things that put you at risk for getting asthma as an adult are ongoing (chronic) wheezing when you were a child and cigarette smoking.footnote 3, footnote 4
Personal and family history
- Gender and age. Women and men seem to have the same risk of getting asthma until they reach their 40s. After 40, women have a higher risk for asthma.
- A family history of allergies and asthma. People who have an allergy and asthma usually have a family history of allergies or asthma.
- Airways that overreact. People who inherit a tendency of the airways to overreact often get asthma.
- A history of allergy. If you have an allergy, you are more likely than others to have asthma. Most children and many adults with asthma have atopic dermatitis, allergies, or both.
Other things that increase your risk
- Cigarette smoking. People who smoke are more likely to get asthma than people who don’t. If you already have asthma and you smoke, it may make your symptoms worse.
- Cigarette smoking during pregnancy. This raises the risk of wheezing in babies. Babies whose mothers smoked during pregnancy also have worse lung function than those whose mothers didn’t smoke.
- Workplace exposure to irritants or allergens. This causes occupational asthma. Irritants or allergens also can make symptoms worse in people who already have asthma.
- Cockroaches. Cockroach droppings in a child’s home have been linked to a higher risk for asthma.footnote 5
- Obesity. Being obese raises your risk for asthma.footnote 6 Weight gain may make asthma worse.
Risk factors that may make asthma worse (triggers)
Triggers that may make asthma worse and may lead to asthma attacks include:
- Infections, such as severe upper respiratory infections (URIs). URIs cause more than half of the asthma attacks in adults.footnote 7
- Allergens, such as dust mites, mold, or pet dander, in people allergic to them.footnote 5
Possible risk factors that need more research
Experts aren’t yet sure:
- About the effect that pets in the home have on getting asthma. A review of several studies found that having a pet cat appeared to protect against asthma, while pet dogs slightly increased the risk of asthma. The effect of other furry pets on the risk of asthma was not clear.footnote 8 If your child already has asthma and allergies to pets, having a pet in the home may make his or her asthma worse.
When to Call a Doctor
Call 911 or other emergency services right away if:
- You are having severe trouble breathing.
Call your doctor now or seek immediate medical care if:
- Your symptoms do not get better after you have followed your asthma action plan.
- You have new or worse trouble breathing.
- Your coughing and wheezing get worse.
- You cough up dark brown or bloody mucus (sputum).
- You have a new or higher fever.
Call your doctor if:
- You need to use quick-relief medicine on more than 2 days a week (unless it is just for exercise).
- You cough more deeply or more often, especially if you notice more mucus or a change in the color of your mucus.
- You have asthma and your peak flow has been getting worse for 2 to 3 days.
If you have not been diagnosed with asthma but have mild asthma symptoms, call your doctor and make an appointment for an evaluation.
Teen asthma
If your teenager has symptoms of asthma, it is important to see a doctor. Many teens with frequent wheezing may have asthma but aren’t diagnosed with the disease. Teens who have asthma but are less likely to be diagnosed are most often:footnote 9
- Girls.
- Smokers, or teens who are exposed to household cigarette smoke.
- Those with low socioeconomic status.
- Those who have allergies.
- African Americans, Native Americans, or Mexican Americans.
Watchful waiting
Watchful waiting is a “wait and see” approach.
Watchful waiting may be appropriate if you follow your asthma action plan and stay within the green zone. Watch your symptoms, and continue to avoid your asthma triggers.
If you have been getting treatment for 1 to 3 months but aren’t improving, ask your doctor if you need to see an asthma specialist.
Who to see
Doctors who can diagnose and treat asthma include:
You may need to see a specialist (allergist or pulmonologist) if you have:
- Severe persistent asthma.
- Other medical conditions that make it hard to treat asthma.
- A need for more education or trouble following your asthma action plan.
- Not met the goals of treatment after several months of therapy.
- Had a life-threatening asthma attack.
- Skin testing for allergies.
- Occupational asthma.
Exams and Tests
A diagnosis of asthma is based on your medical history, a physical exam, and lung function tests.
Lung function tests
Lung function tests can diagnose asthma, show how severe it is, and check for complications.
- Spirometry is the most common test to diagnose asthma. It measures how quickly you can move air in and out of the lungs and how much is moved.
- Testing of daytime changes in peak expiratory flow (PEF) may be done over 1 to 2 weeks. This test is needed when you have symptoms off and on but have normal spirometry test results.
- An exercise or inhalation challenge may be used if the spirometry test results have been normal or near normal but asthma is still suspected. These tests measure how quickly you can breathe in and out after exercise or after using a medicine. An inhalation challenge also may be done using a specific irritant or allergen if your doctor suspects occupational asthma.
Tests for other diseases
Asthma can be hard to diagnose because the symptoms vary widely. And asthma-like symptoms can also be caused by other conditions, such as a viral lung infection or a vocal cord problem. So your doctor may want to do one or more extra tests.
- More lung function tests may be needed if your doctor suspects another lung disease, such as COPD.
- An electrocardiogram (EKG, ECG) might be done to rule out serious conditions with similar symptoms, such as chronic heart failure. This test measures the electrical signals that control the rhythm of your heartbeat.
- A bronchoscopy test can be done to examine the airways for problems such as tumors or foreign bodies. This test uses a long, thin, lighted tube to look at your airways.
- Biopsies of the airways can be done to look for changes that point to asthma.
- A chest X-ray may be used to look for signs of other lung diseases, such as fibrous tissue caused by chronic inflammation (pulmonary fibrosis).
- Blood tests, such as a complete blood count (CBC), may be done to look for signs of an infection or other condition.
Regular checkups
You need to monitor your condition and have regular checkups to keep asthma under control and to review and possibly update your asthma action plan. Checkups are recommended every 1 to 12 months, depending on how well your asthma is controlled.
During checkups, your doctor will ask about information you may have tracked in an asthma diary, such as:
- Whether your symptoms or your peak expiratory flow or both have held steady, improved, or become worse.
- Asthma attacks during exercise or at night.
Based on the results, your asthma category may change, and your doctor may change the medicines you use or how much medicine you use.
Tests to identify triggers
If you have persistent asthma and take medicine every day, your doctor may ask about your exposure to substances (allergens) that cause an allergic reaction. For more information about testing for triggers, see the topic Allergic Rhinitis.
Allergy tests can include skin tests and a blood test. Skin tests are needed if you are interested in immunotherapy, such as allergy shots.
Treatment Overview
It’s important to treat asthma, because even mild asthma can damage your airways.
Know the goals of treatment
By following your treatment plan, you can meet your goals to:footnote 10
- Prevent symptoms.
- Keep your lung function as close to normal as possible.
- Be able to do your normal daily activities, including work, school, exercise, and recreation.
- Prevent asthma attacks.
- Have few or no side effects from medicine.
Follow your asthma action plan
An asthma action plan tells you which medicines to take every day and how to treat asthma attacks. It may include an asthma diary where you record your peak expiratory flow (PEF) or your symptoms, or both. You also can list the cause of your symptoms and what medicines you took for quick relief. This helps you identify triggers that can be changed or avoided. It also lets you be aware of your symptoms and know how to make quick decisions about medicine and treatment. See an example of an asthma action plan( What is a PDF document? ).
Take medicines
You’ll likely take several medicines to control your asthma and to prevent attacks. Your doctor may adjust your medicines depending on how well your asthma is controlled. Medicines include:
- Oral or injected corticosteroids. These medicines may be used to get your asthma under control before you start taking daily medicine. They can also be used to treat any sudden and severe symptoms (asthma attacks), such as shortness of breath.
- Inhaled corticosteroids (controller medicine). These reduce the inflammation in your airways. You take them every day to keep asthma under control and to prevent asthma attacks.
- Short-acting beta2-agonists and anticholinergics (quick-relief medicine). These medicines are used for asthma attacks. Overuse of quick-relief medicine can be harmful.
Inhalers deliver medicine directly to the lungs. To get the best asthma control possible, be sure you know how to use your inhaler. Use a spacer with your inhaler if your doctor recommends it.
Go to checkups
Be sure to monitor your asthma and have regular checkups. Checkups are recommended every 1 to 12 months, depending on how well your asthma is controlled.
Control triggers
Being around asthma triggers increases symptoms. Try to avoid irritants (such as smoke or air pollution) or things that you may be allergic to (such as animal dander). If something at work is causing your asthma or making it worse (occupational asthma), you may need to wear protective gear, switch to some other task or area, or change jobs.
If you have persistent asthma and react to allergens, you may need to have skin testing for allergies. Immunotherapy, such as allergy shots, may help prevent or reduce some allergy symptoms.
Check peak flow if your doctor recommends it
It’s easy to underestimate how severe your symptoms are. You may not notice them until your lungs are functioning at 50% of your personal best peak expiratory flow (PEF).
Measuring PEF is a way to keep track of asthma symptoms at home. It can help you know when your lung function is getting worse before it drops to a dangerously low level. You can do this with a peak flow meter.
Get help for special concerns
Special considerations in treating asthma include:
- Treating other health problems. If you also have other health problems, such as inflammation and infection of the sinuses (sinusitis) or gastroesophageal reflux disease (GERD), you will need treatment for those conditions.
- Managing asthma during pregnancy. If a woman had asthma before becoming pregnant, her symptoms may become better or worse during pregnancy. Pregnant women whose asthma is not well controlled may be at risk for a number of complications.
- Managing exercise-induced asthma. Exercise often causes asthma symptoms. Steps you can take to reduce the risk of this include using medicine 10 to 30 minutes before you exercise.
- Managing asthma before surgery. People who have moderate to severe asthma are at higher risk of having problems during and after surgery than people who don’t have asthma.
- Managing asthma in older adults. Older adults tend to have worse asthma symptoms and a higher risk of death from asthma than younger people. They may also have one or more other health conditions or be taking other medicines that can make asthma symptoms worse.
Know what to do if asthma gets worse
If your asthma isn’t improving, make an appointment with your doctor to:
- Review your asthma diary to see if you have a new or previously unidentified trigger, such as animal dander. Talk to your doctor about how best to avoid triggers.
- Review your medicines to be sure you are using the right ones and are using them correctly.
- Review your asthma action plan to be sure it is still suitable for your condition.
- See if you have a condition with symptoms similar to asthma, such as sinusitis.
- Make sure you are using your inhaler correctly.
If your medicine isn’t controlling airway inflammation, your doctor will first check to see if you are using the inhaler correctly. If you are using it the right way, your doctor may increase the dosage or switch to another medicine. Or he or she may add a medicine to your treatment.
For severe asthma that cannot be controlled with medicines, bronchial thermoplasty may be an option. This treatment is being studied in clinical trials. Heat is applied to the airways to help reduce the thickness of the airways and to help improve the ability to breathe.
Plan for emergencies
If you have a severe asthma attack (the red zone of your asthma action plan), use medicine based on your action plan and talk with a doctor right away about what to do next.
You may have to go to the hospital or an emergency room for treatment. Be sure to tell the emergency staff if you are pregnant.
At the hospital, you will probably receive inhaled beta2-agonists and corticosteroids. You may be given oxygen therapy. Your lung function and condition will be checked. You may need more treatment in the emergency room or a stay in the hospital.
Some people are at increased risk of death from asthma, such as people who have been admitted to an intensive care unit for asthma or who have needed a breathing tube (intubation) for asthma. If you are high-risk, seek medical care early when you have symptoms.
Prevention
Although there is no certain way to prevent asthma, you can reduce airway inflammation and your risk of asthma attacks.
The goal is to reduce the number, length, and severity of asthma attacks. Start by avoiding your asthma triggers. Also be sure to:
- Get a flu vaccine every year. Have your family members get one too.
- Get the pneumococcal vaccine. The vaccine may not prevent pneumonia, but it can prevent some of the serious complications of pneumonia.
- Avoid taking aspirin, ibuprofen, or other similar medicines if they increase your asthma symptoms. Think about using acetaminophen (Tylenol) instead. (Do not give aspirin to anyone younger than 20 because of the risk of Reye syndrome, a rare but serious problem.) Be safe with medicines. Read and follow all instructions on the label.
- Be alert to foods that may cause asthma symptoms. Some people have symptoms after eating processed potatoes, shrimp, nuts, and dried fruit, or after drinking beer or wine. These foods and liquids contain sulfites, which may cause asthma symptoms.
Irritants in the air
Common irritants in the air, such as tobacco smoke and air pollution, can trigger asthma attacks in some people. They include:
- Some household cleaning products. If a cleaning product seems to trigger your asthma, stop using it. Or use another product that doesn’t cause symptoms.
- Air pollution. Consider staying inside when air pollution levels are high. Avoid indoor irritants in the air (such as fumes from gas, oil, or kerosene or wood-burning stoves). Or you may want to use an air filtration unit in your house to reduce the amount of dust and other pollutants.
- Tobacco smoke. If you have asthma, try to avoid being around others who are smoking, and ask people not to smoke in your house. This helps children, too, since exposing young children to secondhand tobacco smoke makes them more likely to get asthma.
Exercise
Exercise is an asthma trigger for some people. If you often have asthma attacks when you exercise, use your inhaler 10 to 30 minutes before you start the activity so you can avoid an attack.
Avoid exercising outdoors in cold weather. If you are outdoors in cold weather, wear a scarf around your face and breathe through your nose.
Living With Asthma
You can control the impact of asthma with an asthma action plan. A good action plan reminds you to take your daily controller medicines and to be aware of your symptoms and triggers. It also tells you how to make quick decisions about medicine and treatment when you need to.
Learn about asthma, and see your doctor
- Educate yourself about asthma. Your doctor may give you a questionnaire to help you find out what you already know about asthma.
- See your doctor regularly to monitor your asthma. How often you’ll need checkups depends on how well your asthma is controlled. Checkups are recommended every 1 to 12 months. Bring your asthma plan to appointments.
- Set goals that relate to your quality of life. Being able to measure your success motivates you to follow your asthma plan consistently. Decide what you want to be able to do. Have nights free of symptoms? Be able to exercise on a regular basis? Feel secure in knowing you can deal with an asthma attack? Work with your doctor to see if your goals are realistic and how to meet them.
- Know your barriers and solutions. What may prevent you from following your plan? These may be physical barriers, such as living far from your doctor or pharmacy. Or you may have emotional barriers, such as fears about asthma, or unrealistic expectations. Discuss your barriers with your doctor, and work to find solutions.
Follow your asthma action plan
- Your asthma action plan describes which controller medicines to take every day to help delay the long-term effects of asthma. The action plan also contains the steps to treat asthma attacks. See an example of an asthma action plan( What is a PDF document? ).
- Use an asthma diary to help manage your asthma. Record your peak expiratory flow or your symptoms, or both. Also list the cause of your symptoms and what medicines you took for quick relief.
Know your asthma triggers
A trigger is anything that can lead to an asthma attack. A trigger can be smoke, air pollution, allergens, some medicines, or even stress. Avoiding triggers will help decrease the chance of having an asthma attack.
In the case of allergy triggers, avoiding them will help control inflammation in the airways. If you have asthma triggered by an allergen, taking allergy medicine may help you manage the allergy. It may limit the allergy’s effect on your asthma.
Take your asthma medicine
Taking medicines is an important part of asthma treatment. But because you may need to take more than one medicine, it can be hard to remember to take them. To help yourself remember, understand the reasons people don’t take their asthma medicines. Then find ways to overcome those obstacles, such as taping a note to your refrigerator.
Check peak flow if your doctor recommends it
It’s easy to underestimate how severe your symptoms are. You may not notice symptoms until your lungs are functioning at 50% of your personal best measurement.
Measuring peak expiratory flow (PEF) is a way to keep track of asthma symptoms at home. Doing this can help you know when your lung function is getting worse before it drops to a dangerously low level. You can do this with a peak flow meter.
Travel
Most people who have asthma can travel freely. But if you travel to remote areas and take part in intense physical activity, such as long hikes, you may be at increased risk for an asthma attack in an area where emergency help may be hard to find.
When traveling, keep your medicine with you, carry the prescription for it, and use it as prescribed. Also carry your asthma action plan so you know what medicines to take every day and what to do if you have an asthma attack.
Give teens extra attention
Teens who have asthma may view the disease as cutting into their independence and setting them apart from their peers. Parents and other adults can offer support and encouragement to help teens stick with a treatment program. It’s important to:
- Help your teen remember that asthma is only one part of life.
- Allow your teen to meet with the doctor alone. This will encourage your teen to become involved in his or her care.
- Work out a daily management plan that allows a teen to continue daily activities, especially sports. Exercise is important for strong lungs and overall health.
- Talk to your teen about the dangers of smoking and drug use.
- Encourage your teen to meet others who have asthma so they can support each other.
Medications
Medicine doesn’t cure asthma. But it is an important part of managing it. Medicines for asthma treatment are used to:
- Prevent and control airway inflammation so you have fewer asthma symptoms.
- Decrease how often you have asthma attacks, how long they last, and how severe they are.
- Treat the attacks as they occur.
Asthma medicines are divided into two groups: those for prevention and long-term control of inflammation and those that provide quick relief for asthma attacks.
- Long-term (controller) medicines are used daily for persistent asthma.
- Quick-relief medicines are used as needed and provide rapid relief of symptoms during asthma attacks.
How to take asthma medicine
Most medicines for asthma are inhaled. Inhaled medicines are used because a specific dose can be given directly to the airways.
Delivery systems include metered-dose and dry powder inhalers and nebulizers.
Doctors recommend using a spacer with an MDI to better deliver the medicine to the lungs. For many people, a spacer makes an MDI easier to use.
Medicine choices
The most important asthma medicines are:
- Inhaled corticosteroids. These are the preferred controller medicines for long-term treatment of asthma. They reduce inflammation of your airways. You take them every day to keep asthma under control and to prevent sudden and severe symptoms (asthma attacks). They include budesonide, fluticasone, and mometasone.
- Oral or injected corticosteroids (systemic corticosteroids). They get your asthma under control before you start taking daily medicine. You may also need these medicines to treat asthma attacks. Oral corticosteroids are used much more than injected corticosteroids. They include methylprednisolone and prednisone.
- Short-acting beta2-agonists for asthma attacks. They relax the airways, allowing you to breathe easier. These quick-relief medicines include albuterol.
There are other long-term medicines for daily treatment. They include:
- Anticholinergics (such as tiotropium) for poorly controlled asthma.
- Leukotriene pathway modifiers (such as montelukast, zafirlukast, and zileuton).
- Long-acting beta2-agonists (such as formoterol and salmeterol). They are always used with an inhaled corticosteroid as a single medicine combination.
- Less commonly, mast cell stabilizers (such as cromolyn) or theophylline.
Other medicines may be given in some cases.
- Magnesium sulfate may be used if asthma does not improve with standard treatment.
- Anticholinergics (such as ipratropium) are sometimes used for severe asthma attacks.
- Your doctor may recommend other medicines if you have severe allergic asthma and the symptoms aren’t relieved by avoiding allergens or by taking standard medicines. Examples include mepolizumab and omalizumab.
A quick-relief medicine, racepinephrine (Asthmanefrin), is available without a prescription. This medicine isn’t used with an inhaler. It comes with an atomizer that delivers the medicine as a mist.
Be safe with medicine. Read and follow all instructions on the label.
The right medicine for you
Medicine treatment for asthma depends on your age and type of asthma, and how well the treatment is controlling your asthma symptoms.
- The least amount of medicine that controls the asthma symptoms is used.
- The amount of medicine and number of medicines are increased in steps. So if asthma isn’t controlled at a low dose of one controller medicine, the dose may be increased. Or another medicine may be added.
- If the asthma has been under control for several months at a certain dose of medicine, the dose may be reduced. This can help find the least amount of medicine that will control the asthma.
- Quick-relief medicine is used to treat asthma attacks. But if you need to use quick-relief medicine a lot, the amount and number of controller medicines may be changed.
Your doctor will work with you to help find the number and dose of medicines that work best.
What to think about
One of the best tools for managing asthma is a daily controller medicine that has a corticosteroid (“steroid”). But some people worry about taking steroid medicines because of myths they’ve heard about them. If you’re making a decision about a steroid inhaler, it helps to know the facts.
At the start of asthma treatment, the number and dosage of medicines are chosen to get the asthma under control. Your doctor may start you at a higher dose within your asthma classification so that the inflammation is controlled right away. After the asthma has been controlled for several months, the dose of the last medicine added is reduced to the lowest possible dose that prevents symptoms. This is known as step-down care. Step-down care is believed to be a better way to control inflammation in the airways than starting at lower doses of medicine and increasing the dose if it is not enough.footnote 11
Because quick-relief medicine quickly reduces symptoms, people sometimes overuse these medicines instead of using the slower-acting long-term medicines. But overuse of quick-relief medicines may have harmful effects, such as reducing how well these medicines will work for you in the future.footnote 12
You may have to take more than one medicine each day to manage your asthma. Help yourself remember when to take each medicine, such as taping a note to your refrigerator to remind yourself.
Tell your doctor about all the medicines you are taking, so he or she can choose asthma medicines that won’t interfere with other medicines.
Some people only have symptoms during certain times of the year (seasonal asthma). If you know when you will most likely have symptoms, start using a medicine to decrease inflammation before the symptoms start.
Other Treatment
Bronchial thermoplasty
If you have severe asthma, bronchial thermoplasty may be an option. This treatment is being studied in clinical trials. For this treatment, bronchoscopy is used to apply heat to the airways. This may help reduce the thickness of the airways and may help improve the ability to breathe.
Immunotherapy
If you have asthma symptoms that are triggered by allergens, your doctor may recommend immunotherapy. For this treatment, you get allergy shots or use pills that have a small amount of certain allergens in them. Your body “gets used to” the allergen, so you react less to it over time. This kind of treatment may help prevent or reduce some allergy symptoms.
For some people, allergy shots reduce asthma symptoms and the need for medicines.footnote 13 But allergy shots don’t work equally well for all allergens. Allergy shots should not be given when asthma is poorly controlled.
Complementary medicine
Complementary medicine is a term used for a wide variety of health care practices that may be used along with standard medical treatment.
Some people have found that mind and body practices such as acupuncture, breathing exercises, and yoga have been helpful for their asthma. But reviewers who have looked at the research say that there isn’t enough scientific evidence to say that complementary practices will help people who have asthma.
Talk with your doctor about any complementary health practice that you would like to try or are already using. Your doctor can help you manage your health better if he or she has the whole picture about your health.
For more information on alternative treatments, see the topic Complementary Medicine.
References
Citations
- McGeady SJ (2004). Immunocompetence and allergy. Pediatrics, 113(4): 1107–1113.
- Silva GE, et al. (2004). Asthma as a risk factor for COPD in a longitudinal study. Chest, 126(1): 59–65.
- Guilbert T, Krawiec M (2003). Natural history of asthma. Pediatric Clinics of North America, 50(3): 524–538.
- Stern DA, et al. (2008). Wheezing and bronchial hyper-responsiveness in early childhood as predictors of newly diagnosed asthma in early adulthood: A longitudinal birth-cohort study. Lancet, 372(9643): 1058–1064.
- Etzel RA (2003). How environmental exposures influence the development and exacerbation of asthma. Pediatrics, 112(1): 233–239.
- Beuther DA, Sutherland ER (2007). Overweight, obesity, and incident asthma: A meta-analysis of prospective epidemiologic studies. American Journal Of Respiratory and Critical Care Medicine, 175(7): 661–666.
- Lemanske RF Jr (2003). Viruses and asthma: Inception, exacerbations, and possible prevention. Proceedings from the Consensus Conference on Treatment of Viral Respiratory Infection-Induced Asthma in Children. Journal of Pediatrics, 142(2, Suppl): S3–S7.
- Takkouche B, et al. (2008). Exposure to furry pets and the risk of asthma and allergic rhinitis: A meta-analysis. Allergy, 63(7): 857–864.
- Yeatts K, et al. (2003). Who gets diagnosed with asthma? Frequent wheeze among adolescents with and without a diagnosis of asthma. Pediatrics, 111(5): 1046–1054.
- Joint Task Force on Practice Parameters (2005). Attaining optimal asthma control: A practice parameter. Journal of Allergy and Clinical Immunology, 116(5): S3–S11. Available online: http://www.allergyparameters.org/file_depot/0-10000000/30000-40000/30326/folder/73825/2005+Asthma+Control.pdf.
- National Institutes of Health (2007). National Asthma Education and Prevention Program Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma (NIH Publication No. 08–5846). Available online: http://www.nhlbi.nih.gov/guidelines/asthma/index.htm.
- Salpeter SR, et al. (2004). Meta-analysis: Respiratory tolerance to regular beta2-agonist use in patients with asthma. Annals of Internal Medicine, 140(10): 802–813.
- Abramson MJ, et al. (2010). Injection allergen immunotherapy for asthma. Cochrane Database of Systematic Reviews (8). Oxford: Update Software.
Other Works Consulted
- Chung KF, et al. (2014). International ERS/ATS guidelines on definition, evaluation and treatment of severe asthma. European Respiratory Journal, 43(2): 343–373. DOI: 10.1183/09031936.00202013. Accessed March 11, 2014.
- Grayson MH, Holtzman MJ (2007). Asthma. In EG Nabel, ed., ACP Medicine, section 14, chap. 19. Hamilton, ON: BC Decker.
- Jaeschke R, et al. (2008). The safety of long-acting beta-agonists among patients with asthma using inhaled corticosteroids. American Journal of Respiratory and Critical Care Medicine, 178(10): 1009–1016.
- Schatz M (2015). Asthma in adults and adolescents. In ET Bope et al., eds., Conn’s Current Therapy 2015, pp. 363–371. Philadelphia: Saunders.
Current as of: June 9, 2019
Author: Healthwise Staff
Medical Review:E. Gregory Thompson, MD – Internal Medicine & Adam Husney, MD – Family Medicine & Kathleen Romito, MD – Family Medicine & Elizabeth T. Russo, MD – Internal Medicine
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.