Cannabis and Cannabinoids (PDQ®): Integrative, alternative, and complementary therapies – Patient Information [NCI]
This information is produced and provided by the National Cancer Institute (NCI). The information in this topic may have changed since it was written. For the most current information, contact the National Cancer Institute via the Internet web site at http://cancer.gov or call 1-800-4-CANCER.
Overview
- Cannabis, also known as marijuana, is a plant grown in many parts of the world. It makes a resin (thick substance) that contains compounds called cannabinoids (see Question 1).
- By federal law, possessing Cannabis is illegal in the United States outside of approved research settings. However, a growing number of states, territories, and the District of Columbia have passed laws to legalize medical marijuana (see Question 1).
- Cannabinoids are chemicals in Cannabis that cause drug -like effects throughout the body, including the central nervous system and the immune system (see Question 2).
- The main psychoactive cannabinoid in Cannabis is delta-9-THC. Another active cannabinoid is cannabidiol (CBD), which may relieve pain, lower inflammation, and decrease anxiety without causing the “high” of delta-9-THC (see Question 2).
- Cannabinoids can be taken by mouth, inhaled, or sprayed under the tongue (see Question 4).
- Cannabis and cannabinoids have been studied for relief of pain, nausea and vomiting, anxiety, and loss of appetite caused by cancer or the side effects of cancer therapies (see Question 6).
- Two cannabinoid drugs (dronabinol and nabilone) are approved by the U.S. Food and Drug Administration (FDA) for the prevention or treatment of nausea and vomiting caused by chemotherapy (see Question 6 and Question 8).
- The FDA has not approved Cannabis or cannabinoids for use as a cancer treatment (see Question 8).
Questions and Answers About Cannabis
Cannabis, also known as marijuana, is a plant first grown in Central Asia that is now grown in many parts of the world. The Cannabis plant makes a resin (thick substance) that contains compounds called cannabinoids. Some cannabinoids are psychoactive (affecting your mind or mood). In the United States, Cannabis is a controlled substance and has been classified as a Schedule I agent (a drug with a high potential for abuse and no accepted medical use).
Clinical trials that study Cannabis for cancer treatment are limited.
By federal law, possessing Cannabis (marijuana) is illegal in the United States unless it is used in approved research settings. However, a growing number of states, territories, and the District of Columbia have passed laws to legalize medical marijuana. (See Question 3).
What are cannabinoids?
Cannabinoids, also known as phytocannabinoids, are chemicals in Cannabis that cause drug-like effects in the body, including the central nervous system and the immune system. The main psychoactive cannabinoid in Cannabis is delta-9-THC. Another active cannabinoid is cannabidiol (CBD), which may relieve pain and lower inflammation without causing the high of delta-9-THC.
Cannabinoids may help treat the side effects of cancer and cancer treatment.
If Cannabis is illegal, how do some cancer patients in the United States use it?
Although federal law prohibits the use of Cannabis, the map below shows the states and territories that have legalized Cannabis for medical purposes. Some other states have legalized only one ingredient in Cannabis, such as cannabidiol (CBD), and these states are not included in the map. Medical marijuana laws vary from state to state.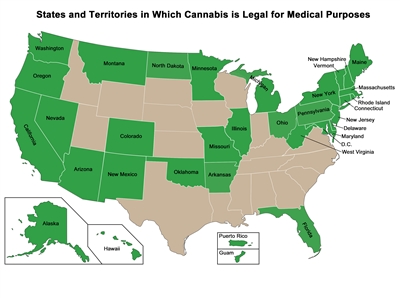
A map showing the U.S. states and territories that have approved the medical use of Cannabis.
How is Cannabis given or taken?
Cannabis may be taken by mouth (in baked products or as an herbal tea) or may be inhaled. When taken by mouth, the main psychoactive ingredient in Cannabis (delta-9-THC) is processed by the liver and changed into a different psychoactive chemical (11-OH-THC).
When Cannabis is smoked and inhaled, cannabinoids quickly enter the bloodstream. The psychoactive chemical (11-OH-THC) is made in smaller amounts than when taken by mouth.
A growing number of clinical trials are studying a medicine made from an extract of Cannabis that contains specific amounts of cannabinoids. This medicine is sprayed under the tongue.
Have any laboratory or animal studies been done using Cannabis or cannabinoids?
In laboratory studies, tumor cells are used to test a substance to find out if it is likely to have any anticancer effects. In animal studies, tests are done to see if a drug, procedure, or treatment is safe and effective in animals. Laboratory and animal studies are done before a substance is tested in people.
Laboratory and animal studies have tested the effects of cannabinoids in laboratory experiments. See the Laboratory/Animal/Preclinical Studies section of the health professional version of Cannabis and Cannabinoids for information on laboratory and animal studies done using cannabinoids.
Have any studies of Cannabis or cannabinoids been done in people?
No ongoing studies of Cannabis as a treatment for cancer in people have been found in the CAM on PubMed database maintained by the National Institutes of Health.
Small studies have been done, but the results have not been reported or suggest a need for larger studies.
- Cannabidiol (CBD) taken by mouth to treat solid tumors that have recurred (come back).
- An oral spray combining 2 cannabinoids (delta-9-THC and CBD) given with temozolomide to treat recurrent glioblastoma multiforme.
- CBD taken by mouth to treat acute graft-versus-host disease in patients who have undergone allogeneic hematopoietic stem cell transplantation.
Cannabis and cannabinoids have been studied as ways to manage side effects of cancer and cancer therapies.
Nausea and vomiting
Cannabis and cannabinoids have been studied in the treatment of nausea and vomiting caused by cancer or cancer treatment:
- Delta-9-THC taken by mouth: Two cannabinoid drugs, dronabinol and nabilone, approved by the U.S. Food and Drug Administration (FDA), are given to treat nausea and vomiting caused by chemotherapy in patients who have not responded to standard antiemetic therapy. Clinical trials have shown that both dronabinol and nabilone work as well as or better than other drugs to relieve nausea and vomiting.
- Oral spray with delta-9-THC and CBD: Nabiximols, a Cannabis extract given as a mouth spray, was shown in a small randomized, placebo-controlled, double-blinded clinical trial in Spain to treat nausea and vomiting caused by chemotherapy.
- Inhaled Cannabis: Ten small trials have studied inhaled Cannabis for the treatment of nausea and vomiting caused by chemotherapy.
Newer drugs given for nausea caused by chemotherapy have not been directly compared with Cannabis or cannabinoids in cancer patients.
There is growing interest in treating children for symptoms such as nausea with Cannabis and cannabinoids, but studies are limited. The American Academy of Pediatrics has not endorsed Cannabis and cannabinoid use because of concerns about its effect on brain development.
Stimulating appetite
The ability of cannabinoids to increase appetite has been studied:
- Delta-9-THC taken by mouth: A clinical trial compared delta-9-THC (dronabinol) and a standard drug (megestrol, an appetite stimulant) in patients with advanced cancer and loss of appetite. Results showed that delta-9-THC did not help increase appetite or weight gain in advanced cancer patients compared with megestrol. However, a clinical trial of patients with HIV /AIDS and weight loss found that those who took delta-9-THC had better appetite and stopped losing weight compared with patients who took a placebo.
- Inhaled Cannabis: There are no published studies of the effect of inhaled Cannabis on cancer patients with loss of appetite.
Pain relief
Cannabis and cannabinoids have been studied in the treatment of pain:
- Vaporized Cannabis with opioids: In a study of 21 patients with chronic pain, vaporized Cannabis given with morphine relieved pain better than morphine alone, while vaporized Cannabis given with oxycodone did not give greater pain relief. Further studies are needed.
- Inhaled Cannabis: Randomized controlled trials of inhaled Cannabis in patients with peripheral neuropathy or other nerve pain found pain was reduced in patients who received inhaled Cannabis compared with those who received placebo.
- Cannabis plant extract: A study of Cannabis extract that was sprayed under the tongue found it helped patients with advanced cancer whose pain was not relieved by strong opioids alone. In another study, patients who were given lower doses of cannabinoid spray showed better pain control and less sleep loss than patients who received a placebo. Control of cancer-related pain in some patients was better without the need for higher doses of Cannabis extract spray or higher doses of their other pain medicines. Adverse events were related to high doses of cannabinoid spray.
- Delta-9-THC taken by mouth: Two small clinical trials of oral delta-9-THC showed that it relieved cancer pain. In the first study, patients had good pain relief, less nausea and vomiting, and better appetite. A second study showed that delta-9-THC could relieve pain as well as codeine. An observational study of nabilone also showed that it relieved cancer pain along with nausea, anxiety, and distress when compared with no treatment. Neither dronabinol nor nabilone is approved by the FDA for pain relief.
Anxiety
Cannabis and cannabinoids have been studied in the treatment of anxiety.
- Inhaled Cannabis: A small case series found that patients who inhaled Cannabis had improved mood, improved sense of well-being, and less anxiety. In another study, 74 patients newly diagnosed with head and neck cancer who were Cannabis users were matched to 74 nonusers. The Cannabis users had markedly lower anxiety or depression and less pain or discomfort than the nonusers. The Cannabis users were also less tired, had more appetite, and reported greater feelings of well-being.
Have any side effects or risks been reported from Cannabis and cannabinoids?
Side effects of cannabinoids can include:
- Fast heartbeat.
- Low blood pressure.
- Muscle relaxation.
- Bloodshot eyes.
- Slowed digestion.
- Dizziness.
- Drowsiness.
- Depression.
- Hallucinations.
- Paranoia.
Both Cannabis and cannabinoids may be addictive. Symptoms of withdrawal from cannabinoids include:
- Being easily annoyed or angered.
- Trouble sleeping.
- Unable to stay still.
- Hot flashes.
- Nausea and cramping (rare).
These symptoms are mild compared with symptoms of withdrawal from opiates and usually go away after a few days.
Studies on risks from Cannabis use
Studies on the risk of various cancers linked to Cannabis smoking have shown the following:
- Lung cancer: Because Cannabis smoke contains many of the same substances as tobacco smoke, there are concerns about how inhaled Cannabis affects the lungs. A cohort study of men in Africa found that there was an increased risk of lung cancer in tobacco smokers who also inhaled Cannabis. A population study of lung cancer patients found that low Cannabis use was not linked to an increased risk of lung cancer or other aerodigestive tract cancers.
- Testicular cancer: A 1970 study interviewed over 49,000 Swedish men aged 19 to 21 years about their personal history of using Cannabis at the time they enlisted in the military and then followed them for up to 42 years. The study did not find a link between those who had “ever” used Cannabis and testicular cancer, but did find that “heavy” use of Cannabis (more than 50 times in a lifetime) was linked to more than twice the risk of testicular cancer. The study was limited by the way data was gathered and did not note whether the testicular cancers were seminoma or nonseminoma types or whether Cannabis use also occurred after enlistment.
- Bladder cancer: A review of bladder cancer rates in Cannabis users and non-users was done in over 84,000 men who took part in the California Men’s Health Study. After more than 16 years of follow-up and adjusting for age, race, ethnic group, and body mass index, rates of bladder cancer were found to be 45% lower in Cannabis users than in men who did not report Cannabis use.
Larger studies that follow patients over time are needed to find if there is a link between Cannabis use and a higher risk of testicular germ cell tumors.
Are Cannabis or cannabinoids approved by the U.S. Food and Drug Administration for use as a cancer treatment or treatment for cancer-related symptoms or side effects of cancer therapy?
The U.S. Food and Drug Administration (FDA) has not approved Cannabis or cannabinoids for use as a cancer treatment.
Cannabis is not approved by the FDA for the treatment of any cancer-related symptom or side effect of cancer therapy.
Two cannabinoids (dronabinol and nabilone) are approved by the FDA for the treatment of nausea and vomiting caused by chemotherapy in patients who have not responded to antiemetic therapy.
Current Clinical Trials
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute’s (NCI’s) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government’s center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about the use of Cannabis and cannabinoids in the treatment of people with cancer. It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary (“Updated”) is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Integrative, Alternative, and Complementary Therapies Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become “standard.” Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI’s website. For more information, call the Cancer Information Service (CIS), NCI’s contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as “NCI’s PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary].”
The best way to cite this PDQ summary is:
PDQ® Integrative, Alternative, and Complementary Therapies Editorial Board. PDQ Cannabis and Cannabinoids. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/about-cancer/treatment/cam/patient/cannabis-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389314]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website’s E-mail Us.
General CAM Information
Complementary and alternative medicine (CAM)—also called integrative medicine—includes a broad range of healing philosophies, approaches, and therapies. A therapy is generally called complementary when it is used in addition to conventional treatments; it is often called alternative when it is used instead of conventional treatment. (Conventional treatments are those that are widely accepted and practiced by the mainstream medical community.) Depending on how they are used, some therapies can be considered either complementary or alternative. Complementary and alternative therapies are used in an effort to prevent illness, reduce stress, prevent or reduce side effects and symptoms, or control or cure disease.
Unlike conventional treatments for cancer, complementary and alternative therapies are often not covered by insurance companies. Patients should check with their insurance provider to find out about coverage for complementary and alternative therapies.
Cancer patients considering complementary and alternative therapies should discuss this decision with their doctor, nurse, or pharmacist as they would any type of treatment. Some complementary and alternative therapies may affect their standard treatment or may be harmful when used with conventional treatment.
Evaluation of CAM Therapies
It is important that the same scientific methods used to test conventional therapies are used to test CAM therapies. The National Cancer Institute and the National Center for Complementary and Integrative Health (NCCIH) are sponsoring a number of clinical trials (research studies) at medical centers to test CAM therapies for use in cancer.
Conventional approaches to cancer treatment have generally been studied for safety and effectiveness through a scientific process that includes clinical trials with large numbers of patients. Less is known about the safety and effectiveness of complementary and alternative methods. Few CAM therapies have been tested using demanding scientific methods. A small number of CAM therapies that were thought to be purely alternative approaches are now being used in cancer treatment—not as cures, but as complementary therapies that may help patients feel better and recover faster. One example is acupuncture. According to a panel of experts at a National Institutes of Health (NIH) meeting in November 1997, acupuncture has been found to help control nausea and vomiting caused by chemotherapy and pain related to surgery. However, some approaches, such as the use of laetrile, have been studied and found not to work and to possibly cause harm.
The NCI Best Case Series Program which was started in 1991, is one way CAM approaches that are being used in practice are being studied. The program is overseen by the NCI’s Office of Cancer Complementary and Alternative Medicine (OCCAM). Health care professionals who offer alternative cancer therapies submit their patients’ medical records and related materials to OCCAM. OCCAM carefully reviews these materials to see if any seem worth further research.
Questions to Ask Your Health Care Provider About CAM
When considering complementary and alternative therapies, patients should ask their health care provider the following questions:
- What side effects can be expected?
- What are the risks related to this therapy?
- What benefits can be expected from this therapy?
- Do the known benefits outweigh the risks?
- Will the therapy affect conventional treatment?
- Is this therapy part of a clinical trial?
- If so, who is the sponsor of the trial?
- Will the therapy be covered by health insurance?
To Learn More About CAM
National Center for Complementary and Integrative Health (NCCIH)
The National Center for Complementary and Integrative Health (NCCIH) at the National Institutes of Health (NIH) facilitates research and evaluation of complementary and alternative practices, and provides information about a variety of approaches to health professionals and the public.
| NCCIH Clearinghouse |
| Post Office Box 7923 Gaithersburg, MD 20898–7923 |
| Telephone: 1-888-644-6226 (toll free) |
| TTY (for deaf and hard of hearing callers): 1-866-464-3615 |
| E-mail: info@nccih.nih.gov |
| Website: https://nccih.nih.gov |
CAM on PubMed
NCCIH and the NIH National Library of Medicine (NLM) jointly developed CAM on PubMed, a free and easy-to-use search tool for finding CAM-related journal citations. As a subset of the NLM’s PubMed bibliographic database, CAM on PubMed features more than 230,000 references and abstracts for CAM-related articles from scientific journals. This database also provides links to the websites of over 1,800 journals, allowing users to view full-text articles. (A subscription or other fee may be required to access full-text articles.)
Office of Cancer Complementary and Alternative Medicine
The NCI Office of Cancer Complementary and Alternative Medicine (OCCAM) coordinates the activities of the NCI in the area of complementary and alternative medicine (CAM). OCCAM supports CAM cancer research and provides information about cancer-related CAM to health providers and the general public via the NCI website.
National Cancer Institute (NCI) Cancer Information Service
U.S. residents may call the Cancer Information Service (CIS), NCI’s contact center, toll free at 1-800-4-CANCER (1-800-422-6237) Monday through Friday from 9:00 am to 9:00 pm. A trained Cancer Information Specialist is available to answer your questions.
Food and Drug Administration
The Food and Drug Administration (FDA) regulates drugs and medical devices to ensure that they are safe and effective.
| Food and Drug Administration |
| 10903 New Hampshire Avenue |
| Silver Spring, MD 20993 |
| Telephone: 1-888-463-6332 (toll free) |
| Website: http://www.fda.gov |
Federal Trade Commission
The Federal Trade Commission (FTC) enforces consumer protection laws. Publications available from the FTC include:
- Who Cares: Sources of Information About Health Care Products and Services
- Fraudulent Health Claims: Don’t Be Fooled
| Consumer Response Center |
| Federal Trade Commission |
| 600 Pennsylvania Avenue, NW |
| Washington, DC 20580 |
| Telephone: 1-877-FTC-HELP (1-877-382-4357) (toll free) |
| TTY (for deaf and hard of hearing callers): 202-326-2502 |
| Website: http://www.ftc.gov |
Last Revised: 2019-06-27
If you want to know more about cancer and how it is treated, or if you wish to know about clinical trials for your type of cancer, you can call the NCI’s Cancer Information Service at 1-800-422-6237, toll free. A trained information specialist can talk with you and answer your questions.
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.

