Degenerative Disc Disease
Topic Overview
What is degenerative disc disease?
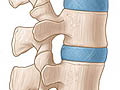
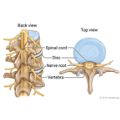
Degenerative disc disease is not really a disease but a term used to describe the normal changes in your spinal discs as you age. Spinal discs are soft, compressible discs that separate the interlocking bones (vertebrae) that make up the spine. The discs act as shock absorbers for the spine, allowing it to flex, bend, and twist. Degenerative disc disease can take place throughout the spine, but it most often occurs in the discs in the lower back (lumbar region) and the neck (cervical region).
The changes in the discs can result in back or neck pain and/or:
- Osteoarthritis, the breakdown of the tissue (cartilage) that protects and cushions joints.
- Herniated disc, an abnormal bulge or breaking open of a spinal disc.
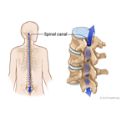
- Spinal stenosis, the narrowing of the spinal canal, the open space in the spine that holds the spinal cord.
These conditions may put pressure on the spinal cord and nerves, leading to pain and possibly affecting nerve function.
What causes degenerative disc disease?
As we age, our spinal discs break down, or degenerate, which may result in degenerative disc disease in some people. These age-related changes include:
- The loss of fluid in your discs. This reduces the ability of the discs to act as shock absorbers and makes them less flexible. Loss of fluid also makes the disc thinner and narrows the distance between the vertebrae.
- Tiny tears or cracks in the outer layer (annulus or capsule) of the disc. The jellylike material inside the disc (nucleus) may be forced out through the tears or cracks in the capsule, which causes the disc to bulge, break open (rupture), or break into fragments.
These changes are more likely to occur in people who smoke cigarettes and those who do heavy physical work (such as repeated heavy lifting). People who are obese are also more likely to have symptoms of degenerative disc disease.
A sudden (acute) injury leading to a herniated disc (such as a fall) may also begin the degeneration process.
As the space between the vertebrae gets smaller, there is less padding between them, and the spine becomes less stable. The body reacts to this by constructing bony growths called bone spurs (osteophytes). Bone spurs can put pressure on the spinal nerve roots or spinal cord, resulting in pain and affecting nerve function.
What are the symptoms?
Degenerative disc disease may result in back or neck pain, but this varies from person to person. Many people have no pain, while others with the same amount of disc damage have severe pain that limits their activities. Where the pain occurs depends on the location of the affected disc. An affected disc in the neck area may result in neck or arm pain, while an affected disc in the lower back may result in pain in the back, buttock, or leg. The pain often gets worse with movements such as bending over, reaching up, or twisting.
The pain may start after a major injury (such as from a car accident), a minor injury (such as a fall from a low height), or a normal motion (such as bending over to pick something up). It may also start gradually for no known reason and get worse over time.
In some cases, you may have numbness or tingling in your leg or arm.
How is degenerative disc disease diagnosed?
Degenerative disc disease is diagnosed with a medical history and physical exam. Your doctor will ask about your symptoms, injuries or illnesses, any previous treatment, and habits and activities that may be causing pain in the neck, arms, back, buttock, or leg. During the physical exam, he or she will:
- Check the affected area’s range of motion and for pain caused by movement.
- Look for areas of tenderness and any nerve-related changes, such as numbness, tingling, or weakness in the affected area, or changes in reflexes.
- Check for other conditions, such as fractures, tumors, and infection.
If your exam reveals no signs of a serious condition, imaging tests, such as an X-ray, are unlikely to help the diagnosis. Imaging tests may be considered when your symptoms develop after an injury, nerve damage is suspected, or your medical history suggests conditions that could affect your spine, such as bone disease, tumors, or infection.
How is it treated?
To relieve pain, put ice or heat (whichever feels better) on the affected area. Ask your doctor if you can take acetaminophen (such as Tylenol) or nonsteroidal anti-inflammatory drugs, such as ibuprofen or naproxen. Your doctor can prescribe stronger medicines if needed. Be safe with medicines. Read and follow all instructions on the label.
If you develop health problems such as osteoarthritis, a herniated disc, or spinal stenosis, you may need other treatments. These include physical therapy and exercises for strengthening and stretching the back. In some cases, surgery may be recommended. Surgery usually involves removing the damaged disc. In some cases, the bone is then permanently joined (fused) to protect the spinal cord. In rare cases, an artificial disc may be used to replace the disc that is removed.
References
Other Works Consulted
- Fast A, Dudkiewicz I (2015). Cervical degenerative disease. In WR Frontera et al., eds., Essentials of Physical Medicine and Rehabilitation, 3rd ed., pp. 12–16. Philadelphia: Saunders.
- Hellum C, et al. (2011). Surgery with disc prosthesis versus rehabilitation in patients with low back pain and degenerative disc: Two year follow-up of randomised study. BMJ. Published online March 25, 2011 (doi:10.1136/bmj.d2786).
- Roh JS, et al. (2005). Degenerative disorders of the lumbar and cervical spine. Orthopedic Clinics of North America, 36(2005): 255–262.
- Schaufele MK, Tate JL (2015). Lumbar degenerative disease. In WR Frontera et al., eds., Essentials of Physical Medicine and Rehabilitation, 3rd ed., pp. 225–232. Philadelphia: Saunders.
Credits
Current as ofJune 26, 2019
Author: Healthwise Staff
Medical Review: William H. Blahd, Jr., MD, FACEP – Emergency Medicine
E. Gregory Thompson, MD – Internal Medicine
Adam Husney, MD – Family Medicine
Kathleen Romito, MD – Family Medicine
Kenneth J. Koval, MD – Orthopedic Surgery, Orthopedic Trauma
Current as of: June 26, 2019
Author: Healthwise Staff
Medical Review:William H. Blahd, Jr., MD, FACEP – Emergency Medicine & E. Gregory Thompson, MD – Internal Medicine & Adam Husney, MD – Family Medicine & Kathleen Romito, MD – Family Medicine & Kenneth J. Koval, MD – Orthopedic Surgery, Orthopedic Trauma
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.