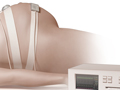
Electronic Fetal Heart Monitoring
Test Overview
Electronic fetal heart monitoring is done during pregnancy, labor, and delivery. It keeps track of the heart rate of your baby (fetus). It also checks the duration of the contractions of your uterus. Your baby’s heart rate is a good way to tell if your baby is doing well or may have some problems.
Two types of monitoring can be done: external and internal.
External monitoring
You may have external monitoring at different times during your pregnancy. Sometimes it’s done during labor.
External monitoring can be done by listening to your baby’s heartbeat with a special stethoscope. More often, it is done using two flat devices (sensors). They are held in place with elastic belts on your belly. One sensor uses reflected sound waves (ultrasound) to keep track of your baby’s heart rate. The other sensor measures how long your contractions last. The sensors are connected to a machine that records the details. Your baby’s heartbeat may be heard as a beeping sound or printed out on a chart. How often you have contractions and how long they last may be printed on a chart.
External monitoring is used for a nonstress test. This test records your baby’s heart rate while your baby is moving and not moving. A nonstress test may be done with a fetal ultrasound to check the amount of amniotic fluid.
External monitoring is also done for a contraction stress test. This test records changes in your baby’s heart rate when you have contractions. It may be done to check on your baby’s health if your baby does not move enough during a nonstress test. It may help predict whether your baby can handle the stress of labor and vaginal delivery.
Sometimes external monitoring is done remotely. This is called telemetry. It allows you to be checked without being hooked up to a machine. At some hospitals, the sensors can send the details about your baby’s heart rate and your contractions to a remote monitor. This monitor is usually at a nurse’s station. Using a remote monitor allows you to walk around freely.
Internal monitoring
Internal monitoring is done during labor. It can be done only after your cervix has dilated to at least 2 centimeters (cm). Your amniotic sac must have ruptured as well. After it is started, it is continued until delivery.
For internal monitoring, a sensor is strapped to your thigh. A thin wire (electrode) from the sensor is put through your cervix into your uterus. The electrode is then attached to your baby’s scalp. Your baby’s heartbeat may be heard as a beeping sound or printed out on a chart.
A small tube that measures contractions may be placed in your uterus next to your baby. The strength and timing of your contractions is often printed out on a chart.
Internal monitoring is more exact than external monitoring for keeping track of your baby’s heart rate and your contractions.
Why It Is Done
External fetal heart monitoring
This type of monitoring is done to:
- Keep track of your baby’s heart rate.
- Measure how often you have contractions and how long they last.
- Find out if you are having preterm labor.
- Check on your baby’s health if your doctor thinks there may be problems. External fetal heart monitoring will be done during a nonstress test to check your baby’s heart rate while at rest and while moving. If your baby does not move during this test, more tests will be needed.
- Check your placenta to make sure that it is giving your baby enough oxygen. If a stress test shows that your baby is not getting enough oxygen, your doctor can decide about the safest way to deliver. If the test shows that your baby may be in danger, your doctor may suggest starting (inducing) labor early. Or your doctor may talk to you about a cesarean section (C-section).
- Check your baby’s health if your baby has not been growing normally. (This is called delayed fetal growth.) Monitoring may also be done if you have diabetes or high blood pressure or if you are over 41 weeks pregnant.
Internal fetal heart monitoring
This type of monitoring is done to:
- Find out if the stress of labor is putting your baby’s health at risk.
- Measure the strength and length of your labor contractions.
How To Prepare
You may be asked to eat a meal shortly before you have a nonstress test. When you digest food, it often causes a baby to move more.
If you smoke, you will be asked to stop smoking for 2 hours before external monitoring. Smoking causes a baby to be less active.
How It Is Done
External monitoring can be done at any time after 20 weeks of pregnancy. Internal monitoring is used only when you are in labor and your amniotic sac has broken. If it is needed and your amniotic sac has not broken, your doctor may break the sac to start the test.
Sometimes both types of monitoring will be done at the same time. Your baby’s heart rate may be checked with an internal sensor, and your contractions may be checked with an external sensor.
External monitoring
For external monitoring, you may lie on your back or left side. Two belts with sensors attached will be placed around your belly. Gel may be applied to provide good contact between the heart rate sensors and your skin. The sensors are attached with wires to a recording device. This device can show or print out a record of your baby’s heart rate and the duration of contractions. The position of the heart rate monitor may be changed now and then as your baby moves.
For a nonstress test, you may be asked to push a button on the machine every time your baby moves or you have a contraction. Your baby’s heart rate is recorded. Then it’s compared to the record of movement or your contractions. This test usually lasts about 30 minutes.
Internal monitoring
For internal monitoring, you will usually lie on your back or left side. A thin wire (electrode) will be put through your cervix and attached to your baby’s scalp. A small tube is also put in your uterus. The tube connects to a device that monitors your contractions.
A belt is placed around your upper leg to keep the monitor in place. The electrode and the tube are attached with wires to a recording device. It can show or print out a record of your baby’s heart rate and the strength and length of your contractions.
How It Feels
Lying on your back (or side) may not be comfortable if you are having contractions. The belts that hold the monitors in place may feel tight.
You may be able to change position or move around more during internal monitoring than during external monitoring.
You may have some discomfort when the internal monitor is put into your uterus.
Risks
Electronic fetal monitoring may be linked to an increase in cesarean deliveries. It may also be linked to the use of a vacuum or forceps during delivery.footnote 1
There is a slight risk of infection for your baby when internal monitoring is done.
Results
Electronic fetal heart monitoring is done during pregnancy, labor, and delivery. It keeps track of the heart rate of your baby (fetus). It also checks the duration of the contractions of your uterus. The results are usually ready right away.
|
Normal: |
Your baby’s heart rate is 110 to 160 beats per minute. |
|
Your baby’s heart rate increases when he or she moves and when your uterus contracts. |
|
|
Your baby’s heart rate drops during a contraction but quickly goes back to normal after the contraction is over. |
|
|
Uterine contractions during labor are strong and regular. |
|
|
Abnormal: |
Your baby’s heart rate is less than 110 beats per minute. |
|
Your baby’s heart rate is more than 160 beats per minute. |
|
|
During a nonstress test, your baby’s heart rate does not increase by 15 beats per minute or it drops far below its baseline rate after he or she moves. |
|
|
Uterine contractions are weak or irregular during labor. |
Fetal monitoring can’t find every type of problem, such as birth defects. A normal result does not guarantee that your baby is healthy.
What Affects the Test
You may not be able to have the test, or the results may not be helpful, if:
- You smoke cigarettes or use other tobacco products.
- You drink or eat large amounts of caffeine. (For example, you drink several cups of strong coffee.)
- There are extra noises such as your heartbeat or your stomach rumbling.
- Your baby is sleeping during a nonstress test.
- There are problems with how an external monitoring device is placed. This can happen if:
- Your baby moves a lot during the test.
- You are pregnant with more than one baby.
- You are overweight.
What To Think About
- Not everyone feels the same about fetal monitoring.
- Some mothers think that it is not needed and it gets in the way of the natural birthing process.
- Other mothers think that it is calming. This may be true if they had problems with earlier pregnancies.
- Monitoring throughout labor (continuous) is more likely to be useful for high-risk pregnancies. For low-risk pregnancies, monitoring from time to time during labor (intermittent) works just as well.
- If your baby seems to be having problems, a blood sample may be taken from a small blood vessel (capillary) in the scalp. The blood sample can help the doctor see if your baby is getting enough oxygen.
- Your baby may move more if you drink juice or eat before a nonstress test. This may make the test results more useful.
- Sometimes other methods (such as ringing a bell near the uterus) are used to cause changes in your baby’s heart rate.
- External fetal heart monitoring is used during other tests of a baby’s health. Examples include a nonstress test, a contraction stress test, and a biophysical profile.
References
Citations
- American College of Obstetricians and Gynecologists (2009, reaffirmed 2015). Intrapartum fetal heart rate monitoring: Nomenclature, interpretation, and general management principles. ACOG Practice Bulletin No. 106. Obstetrics and Gynecology, 114(1): 192–202.
Other Works Consulted
- American College of Obstetricians and Gynecologists (2010). Management of intrapartum fetal heart rate tracings. ACOG Practice Bulletin No. 116. Obstetrics and Gynecology, 116(5): 1232–1240.
- Fischbach F, Dunning MB III (2015). A Manual of Laboratory and Diagnostic Tests, 9th ed. Philadelphia: Wolters Kluwer Health.
Credits
Current as ofMay 29, 2019
Author: Healthwise Staff
Medical Review: Sarah A. Marshall, MD – Family Medicine
E. Gregory Thompson, MD – Internal Medicine
Kathleen Romito, MD – Family Medicine
Adam Husney, MD – Family Medicine
William M. Gilbert, MD – Maternal and Fetal Medicine
Femi Olatunbosun, MB, FRCSC, FACOG – Obstetrics and Gynecology, Reproductive Endocrinology
Current as of: May 29, 2019
Author: Healthwise Staff
Medical Review:Sarah A. Marshall, MD – Family Medicine & E. Gregory Thompson, MD – Internal Medicine & Kathleen Romito, MD – Family Medicine & Adam Husney, MD – Family Medicine & William M. Gilbert, MD – Maternal and Fetal Medicine & Femi Olatunbosun, MB, FRCSC, FACOG – Obstetrics and Gynecology, Reproductive Endocrinology
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.