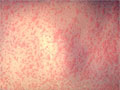
Measles (Rubeola)
Topic Overview
What is measles?
Measles is a very contagious (easily spread) infection that causes a rash all over your body. It is also called rubeola or red measles.
The measles vaccine protects against the illness. This vaccine is part of the MMR (measles, mumps, and rubella) and MMRV (measles, mumps, rubella, and varicella [chickenpox]) vaccines. Most children get the vaccine as part of their regular shots. This is why measles is rare in the United States and Canada.
What causes measles?
Measles is caused by a virus. It is spread when an infected person coughs, sneezes, or shares food or drinks. The measles virus can travel through the air. This means that you can get measles if you are near someone who has the virus even if that person doesn’t cough or sneeze directly on you.
You can spread the virus to others from 4 days before the rash starts until 4 days after the rash appeared. The virus is most often spread when people first get sick, before they know they have it.
If you have had measles, you can’t get it again. Most people born before 1957 have had measles.
What are the symptoms?
The first symptoms of measles are like a bad cold—a high fever, a runny nose, sneezing, a sore throat, and a hacking cough. The lymph nodes in your neck may swell. You also may feel very tired and have diarrhea and red, sore eyes. As these symptoms start to go away, you will get red spots inside your mouth, followed by a rash all over your body.
When adults get measles, they usually feel worse than children who get it.
It usually takes about 7 to 18 days to get symptoms after you have been around someone who has measles. This is called the incubation period.
How is measles diagnosed?
If you think you have measles, call ahead and explain your symptoms before you go to a doctor’s office.
After you’ve had an exam, your doctor may order a blood test and/or viral culture if he or she suspects that you have measles.
How is it treated?
Measles usually gets better with home care. You can take medicine to lower your fever, if needed. Read and follow all instructions on the label. Also, get plenty of rest and drink lots of fluids. Stay away from other people as much as you can so that you don’t spread the disease. Anyone who has measles should stay out of school, day care, work, and public places until at least 4 days after the rash first appeared.
Your doctor may suggest vitamin A supplements if your child has measles.
Most people get better within 2 weeks. But measles can sometimes cause dangerous problems, such as lung infection (pneumonia) or brain swelling (encephalitis). In rare cases, it can even cause seizures or meningitis.
If you have been exposed to measles and you have not had the vaccine, you may be able to prevent the infection by getting immunoglobulin (IG) or the measles vaccine as soon as possible. Babies who are younger than 12 months, pregnant women, and people who have impaired immune systems that can’t fight infection may need to get IG if they are exposed to measles.
Why is prevention important?
Getting your child vaccinated is important, because measles can sometimes cause serious problems.
False claims in the news have made some parents concerned about a link between autism and vaccines. But studies have found no link between vaccines and autism.
Measles is one of the most contagious diseases. Outbreaks can easily occur. For instance, a person from another country may have measles and not know it yet. If that person travels outside his or her own country, he or she could spread measles to people who are not immune. Also, if you travel to another country and you are not immune to measles, you may be at risk.
If you don’t know whether you’re immune to measles and you plan to travel, check with your doctor or local health clinic to see whether you should get the vaccine before you travel.
References
Citations
- Taylor LE, et al. (2014). Vaccines are not associated with autism: An evidence-based meta-analysis of case-control and cohort studies. Vaccines, 32(29): 3623–3629.
Other Works Consulted
- American Academy of Pediatrics (2012). Measles. In LK Pickering et al., eds., Red Book: 2012 Report of the Committee on Infectious Diseases, 29th ed., pp. 489–499. Elk Grove Village, IL: American Academy of Pediatrics.
- Centers for Disease Control and Prevention (2013). Prevention of measles, rubella, congenital rubella syndrome, and mumps, 2013: Summary recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR, 62(RRO4): 1–34. Also available online: http://www.cdc.gov/mmwr/preview/mmwrhtml/rr6204a1.htm.
- Cherry JD (2009). Measles virus. In RD Feigin et al., eds., Feigin and Cherry’s Textbook of Pediatric Infectious Diseases, 6th ed., vol. 2, pp. 2427–2451. Philadelphia: Saunders Elsevier.
- Elliman D, et al. (2009). Measles, mumps, and rubella: Prevention, search date July 2007. Online version of BMJ Clinical Evidence: http://www.clinicalevidence.com.
- Mason WH (2011). Measles. In RM Kliegman et al., eds., Nelson Textbook of Pediatrics, 19th ed., pp. 1069–1075. Philadelphia: Saunders.
- Perry RT, Orenstein WA (2006). Measles. In FD Burg et al., eds., Current Pediatric Therapy, 18th ed., pp. 786–790. Philadelphia: Saunders Elsevier.
Current as of: December 12, 2018
Author: Healthwise Staff
Medical Review:John Pope MD – Pediatrics & Kathleen Romito MD – Family Medicine & E. Gregory Thompson MD – Internal Medicine & Adam Husney MD – Family Medicine & Christine Hahn MD – Epidemiology
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.