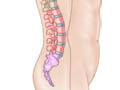
Spondylolisthesis
Topic Overview
What is spondylolisthesis?
Spondylolisthesis is a condition in which one bone in your back (vertebra) slides forward over the bone below it. It most often occurs in the lower spine (lumbosacral area). In some cases, this may lead to your spinal cord or nerve roots being squeezed. This can cause back pain and numbness or weakness in one or both legs. In rare cases, it can also lead to losing control over your bladder or bowels. See a doctor right away if you begin losing bladder or bowel control.
Sometimes when a vertebra slips out of place, you may have no symptoms at all or no symptoms until years later. Then, you may have pain in your low back or buttock. Muscles in your leg may feel tight or weak. You may even limp.
What causes spondylolisthesis?
The bones in your spine come together at several small joints that keep the bones lined up while still allowing them to move. Spondylolisthesis is caused by a problem with one or more of these small joints that allows one bone to move out of line.
Spondylolisthesis may be caused by any of a number of problems with the small joints in your back. You could have:
- A defective joint that you’ve had since birth (congenital).
- A joint damaged by an accident or other trauma.
- A vertebra with a stress fracture caused from overuse of the joint.
- A joint damaged by an infection or arthritis.
Spondylolisthesis affects children and teens involved in sports. Some sports, such as gymnastics or weight lifting, can overuse back bones to the point of causing stress fractures in vertebrae, which can result in spondylolisthesis.
Older adults can develop spondylolisthesis, because wear and tear on the back leads to stress fractures. It can also occur without stress fractures when the disc and joints are worn down and slip out of place.
What are the symptoms?
Symptoms of spondylolisthesis may include:
- Back or buttock pain.
- Pain that runs from the lower back down one or both legs.
- Numbness or weakness in one or both legs.
- Difficulty walking.
- Leg, back, or buttock pain that gets worse when you bend over or twist.
- Loss of bladder or bowel control, in rare cases.
Sometimes spondylolisthesis causes no symptoms at all.
How is spondylolisthesis diagnosed?
Your doctor will look at X-rays of your back if he or she suspects you have spondylolisthesis. X-rays will show if any of the vertebrae in your back have fractures or cracks and have slipped out of place. You could also have a CT scan or an MRI to pinpoint the damage and help guide treatment.
How is it treated?
Treatment for spondylolisthesis begins with stopping any physical activity that may have led to vertebrae damage. To help relieve pain, ask your doctor if you can take nonsteroidal anti-inflammatory drugs, including ibuprofen (such as Advil) or naproxen (such as Aleve). Acetaminophen (such as Tylenol) can also help with pain. Be safe with medicines. Read and follow all instructions on the label.Do not give aspirin to anyone younger than 20 because of the risk of Reye syndrome, a serious illness.
Doctors often suggest physical therapy to build up stomach and back muscles (core strengthening). In overweight people, weight loss may also help.
When pain is extreme or bones continue to move, or if there is nerve root or spinal cord damage related to the spondylolisthesis, surgery can sometimes help. Surgery may be done to remove bone or other tissue to take pressure off the spinal cord or nerves (decompression). Or surgery may be done to fuse the bones in position. Sometimes both decompression and fusion are done during the same surgery. After any of these surgeries, you may need to wear a cast or back brace for a while. Later, rehabilitation therapy will help make your muscles stronger and movement easier.
References
Other Works Consulted
- Kanayama M, et al. (2007). A minimum 10-year follow-up of posterior dynamic stabilization using Graf artificial ligament. Spine, 32(18): 1992–1996.
- Tay BKB, et al. (2014). Disorders, diseases, and injuries of the spine. In HB Skinner, PJ McMahon, eds., Current Diagnosis and Treatment in Orthopedics, 5th ed., pp. 156–229. New York: McGraw-Hill.
Current as of: June 26, 2019
Author: Healthwise Staff
Medical Review:William H. Blahd, Jr., MD, FACEP – Emergency Medicine & Adam Husney, MD – Family Medicine & E. Gregory Thompson, MD – Internal Medicine & Kathleen Romito, MD – Family Medicine
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.