Vaginal Fistula
Topic Overview
What is a vaginal fistula?
A fistula is a passage or hole that has formed between:
- Two organs in your body.
- An organ in your body and your skin.
A fistula that has formed in the wall of the vagina is called a vaginal fistula.
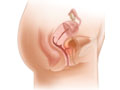
- A vaginal fistula that opens into the urinary tract is called a vesicovaginal fistula.
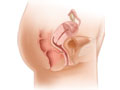
- A vaginal fistula that opens into the rectum is called a rectovaginal fistula.
- A vaginal fistula that opens into the colon is called a colovaginal fistula.
- A vaginal fistula that opens into the small bowel is called a enterovaginal fistula.
See pictures of a vesicovaginal fistula and a rectovaginal fistula.
What causes a vaginal fistula?
A vaginal fistula starts with some kind of tissue damage. After days to years of tissue breakdown, a fistula opens up.
A vaginal fistula sometimes happens after:
- Surgery of the back wall of the vagina, the perineum, anus, or rectum. Open hysterectomy is linked to most vesicovaginal tract fistulas.
- Radiation treatment for pelvic cancer.
- A period of inflammatory bowel disease (including Crohn’s disease and ulcerative colitis) or diverticulitis.
- A deep tear in the perineum or an infected episiotomy after childbirth.
In areas where women have no health care nearby, vaginal fistulas are much more common. After days of pushing a baby that does not fit through the birth canal, very young mothers can have severe vaginal, bladder, or rectal damage, sometimes causing fistulas.
What are the symptoms?
A vaginal fistula is usually painless. But a fistula lets urine or feces pass into your vagina. This is called incontinence. And it can cause soiling problems that you cannot control.
- If you have a vesicovaginal fistula, you most likely have fluid leaking or flowing out of your vagina.
- If you have a rectovaginal, colovaginal, or enterovaginal fistula, you most likely have foul-smelling discharge or gas coming from your vagina.
- Your genital area may get infected or sore.
How is a vaginal fistula diagnosed?
Your symptoms are the most clear signs of a vaginal fistula. Your doctor will want to talk about your symptoms and about any surgery, trauma, or disease that could have caused a fistula. For a physical exam, your doctor will use a speculum to look at the vaginal walls. You may have other tests, such as:
- The use of dye in the vagina (and maybe the bladder or rectum) to find all signs of leakage.
- Urinalysis to check for infection.
- Blood test (complete blood count) to check for signs of infection in your body.
Your doctor may also use an X-ray, endoscope or MRI to get a clear look and check for all possible tissue damage.
How is it treated?
If you have a vaginal fistula, you will most likely need surgery to repair it. Before surgery, your doctor will see whether the tissue is healthy or needs to heal first.
- You may need medicine or wound care to heal the tissue before surgery.
- If you have inflammatory bowel disease, your doctor will not do surgery during a symptom flare.
- If you have a large rectovaginal fistula, you may first have a colostomy. This is to keep the fistula clear for the surgery. After the fistula repair heals, the colostomy is taken out.
After fistula repair surgery, be sure to follow your doctor’s instructions. See your doctor right away if you have signs of infection, such as a fever, tenderness, swelling, or redness.
References
Other Works Consulted
- Katz VL (2012). Postoperative counseling and management. In GM Lentz et al., eds., Comprehensive Gynecology, 6th ed., pp. 583–621. Philadelphia: Mosby.
- Lentz GM (2012). Anatomic defects of the abdominal wall and pelvic floor. In GM Lentz et al., eds., Comprehensive Gynecology, 6th ed., pp. 453–474. Philadelphia: Mosby Elsevier.
- Wong M, Ozel B (2010). Fistulae. In Management of Common Problems in Obstetrics and Gynecology, 5th ed., pp. 328–332. Chichester, UK: Wiley-Blackwell.
Current as of: February 19, 2019
Author: Healthwise Staff
Medical Review:Sarah A. Marshall, MD – Family Medicine & Kathleen Romito, MD – Family Medicine & Martin J. Gabica, MD – Family Medicine & Deborah A. Penava, MD, FRCSC, MPH – Obstetrics and Gynecology
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.