Biophysical Profile (BPP)
Test Overview
A biophysical profile (BPP) test measures the health of your baby (fetus) during pregnancy. A BPP test may include a nonstress test with electronic fetal heart monitoring and a fetal ultrasound. The BPP measures your baby’s heart rate, muscle tone, movement, breathing, and the amount of amniotic fluid around your baby.
A BPP is commonly done in the last trimester of pregnancy. If there is a chance that your baby may have problems during your pregnancy (high-risk pregnancy), a BPP may be done by 32 to 34 weeks or earlier. Some women with high-risk pregnancies may have a BPP test every week or twice a week in the third trimester.
Why It Is Done
A biophysical profile (BPP) test is done to:
- Learn about and keep track of your baby’s health. Special ultrasound methods are used to keep track of movement, increases in heart rate with movement (nonstress test), muscle tone, breathing rate, and the amount of amniotic fluid surrounding your baby. If these five areas are within a normal range, your baby is considered to be in good health.
- Check on your baby’s health if you have:
- Hyperthyroidism.
- Bleeding problems.
- Lupus.
- Chronic kidney disease.
- Type 1 diabetes or gestational diabetes.
- High blood pressure (hypertension).
- Preeclampsia.
- A small amount of amniotic fluid (oligohydramnios) or too much amniotic fluid (polyhydramnios).
- A multiple pregnancy (such as twins or triplets).
- A pregnancy that has gone past your due date, between 40 and 42 weeks.
How To Prepare
You may need a full bladder for the test. If so, you will be asked to drink water or other liquids just before the test and to avoid urinating before or during the test. Usually women in the third trimester do not need to have a full bladder.
If you smoke, you will be asked to stop smoking for 2 hours before the external monitoring test because smoking decreases your baby’s activity.
Talk to your doctor about any concerns you have regarding the need for the test, its risks, how it will be done, or what the results may mean. To help you understand the importance of this test, fill out the medical test information form( What is a PDF document? ).
How It Is Done
Most often, a biophysical profile (BPP) is performed by your obstetrician. But it may be done by an ultrasound technologist or radiologist. A BPP can be done in your doctor’s office, hospital, or clinic.
A nonstress test with electronic fetal heart monitoring and a fetal ultrasound are done as part of a biophysical profile. A nonstress test helps check the baby’s health by looking at the baby’s heart rate with movement.
Some doctors may use a modified biophysical profile, which combines a nonstress test and measurements of the amniotic fluid.
Nonstress test
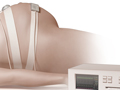
External fetal heart monitoring records your baby’s heart rate while your baby is moving and not moving. It is usually done just before a fetal ultrasound.
External monitoring is done using two flat devices (sensors) held in place with elastic belts on your belly. One sensor uses reflected sound waves (ultrasound) to keep track of your baby’s heart rate. The other sensor measures the duration of your contractions. The sensors are connected to a machine that records the information. Your baby’s heartbeat may be heard as a beeping sound or printed out on a chart.
If your baby moves or you have a contraction, you may be asked to push a button on the machine. Your baby’s heart rate is recorded and compared to the record of movement or your contractions. This test usually lasts about 30 minutes.
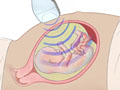
Fetal ultrasound
Often you do not need to remove your clothes for the ultrasound test; you can lift your shirt and push down the waistband of your skirt or pants. If you are wearing a dress, you will be given a cloth or paper covering to use during the test.
- You may need to have a full bladder. You may be asked to drink 4 to 6 glasses of liquid, usually juice or water, about an hour before the test. A full bladder helps transmit sound waves and pushes the intestines out of the way of the uterus. This makes the ultrasound picture clearer.
- You will not be able to urinate until the test is over. But tell the ultrasound technologist if your bladder is so full that you are in pain.
- If an ultrasound is done during the later part of pregnancy, a full bladder may not be needed. The growing fetus will push the intestines out of the way.
- You will lie on your back on a padded examination table. If you become short of breath or lightheaded while lying on your back, your upper body may be raised or you may be turned on your side.
- A gel will be spread on your belly.
- A small, handheld instrument called a transducer will be pressed against the gel on your skin and moved across your abdomen several times. You may watch the monitor to see the picture of the fetus during the test.
When the test is finished, the gel is cleaned off of your skin. You can urinate as soon as the test is done. Transabdominal ultrasound takes about 30 to 60 minutes.
Ultrasound technologists are trained to gather images of your fetus but can’t tell you whether it looks normal or not. Your health professional will share this information with you after the ultrasound images have been reviewed by a radiologist or perinatologist.
How It Feels
Lying on your back (or side) during the test may be uncomfortable. During a fetal ultrasound, you may have a feeling of pressure in your bladder. The gel may feel cool when it is first applied to your stomach. You will feel a light pressure from the transducer as it passes over your abdomen.
Risks
There is very little chance of either the mother or the baby having a problem from a biophysical profile (BPP). But you may feel anxious if the ultrasound reveals a problem with your pregnancy or baby. A nonstress test may falsely show distress in a baby that is actually healthy.
Results
A biophysical profile (BPP) test measures the health of your baby (fetus) during pregnancy. The results are scores on five measurements in a 30-minute observation period. Each measurement has a score of 2 points if normal and 0 points if not normal.
Some BPPs do not include all the measurements. When all five measurements are taken, a score of 8 or 10 points means that your baby is healthy. A score of 6 or 8 points means that you may need to be retested in 12 to 24 hours. A score of 4 or less may mean the baby is having problems. Further testing will be recommended.
What Affects the Test
Reasons you may not be able to have the test or why the results may not be helpful include:
- The baby is in a position that makes doing an ultrasound difficult.
- Being unable to lie still throughout the procedure, which can cause the picture of your baby to be unclear.
- Being overweight, which may make it hard to correctly position the external monitoring device.
- An infection in either you or your baby.
- Low (hypoglycemia) or high (hyperglycemia) blood sugar levels.
- Taking medicine, such as magnesium sulfate.
- Steroids given to help the baby’s lungs mature.
- Using alcohol or illegal drugs, such as cocaine.
- In rare cases, stool (feces) or air in the intestines or rectum interfering with the fetal ultrasound.
What To Think About
- A biophysical profile includes a nonstress test with electronic fetal heart monitoring and a fetal ultrasound.
- More tests, such as a contraction stress test, may be recommended if your results are not normal. To learn more, see the topic Contraction Stress Test.
- If there is a chance that you or your baby may have problems during your pregnancy, you may have a biophysical profile test every week or twice a week during the last 12 weeks of your pregnancy. Your chances of having problems may be higher if you have:
- Certain medical conditions, such as high blood pressure, kidney disease, diabetes, preeclampsia, or autoimmune diseases.
- A history of a stillbirth or preeclampsia.
- A history of Rh incompatibility.
- A history of early labor, prelabor rupture of membranes (PROM), or placenta problems.
- A baby who seems small for the length of the pregnancy or is not growing (intrauterine growth retardation or restriction).
- A biophysical profile may be done after an injury, such as a car crash or fall. Your doctor may recommend more BPP tests during the rest of your pregnancy.
References
Other Works Consulted
- American College of Obstetricians and Gynecologists (1999, reaffirmed 2009). Antepartum fetal surveillance. ACOG Practice Bulletin No. 9. Obstetrics and Gynecology, 94(4): 1–11.
- Fischbach F, Dunning MB III (2015). A Manual of Laboratory and Diagnostic Tests, 9th ed. Philadelphia: Wolters Kluwer Health.
- Pagana KD, Pagana TJ (2014). Mosby’s Manual of Diagnostic and Laboratory Tests, 5th ed. St. Louis: Mosby.
Current as of: May 29, 2019
Author: Healthwise Staff
Medical Review:Sarah Marshall MD – Family Medicine & Kathleen Romito MD – Family Medicine & Adam Husney MD – Family Medicine & William Gilbert MD – Maternal and Fetal Medicine & Femi Olatunbosun MB, FRCSC – Obstetrics and Gynecology
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.