Gout
Topic Overview
What is gout?
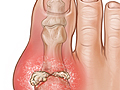
Gout is a kind of arthritis. It can cause an attack of sudden burning pain, stiffness, and swelling in a joint, usually a big toe. These attacks can happen over and over unless gout is treated. Over time, they can harm your joints, tendons, and other tissues. Gout is most common in men.
What causes gout?
Gout is caused by too much uric acid in the blood. Most of the time, having too much uric acid isn’t harmful. Many people with high levels in their blood never get gout. But when uric acid levels in your blood are too high, the uric acid may form hard crystals in your joints.
Your chances of getting gout are higher if you are overweight, drink too much alcohol, or eat too much meat and fish that are high in chemicals called purines. Some medicines, such as water pills (diuretics), can also bring on gout.
What are the symptoms?
The most common sign of gout is a nighttime attack of swelling, tenderness, redness, and sharp pain in your big toe. You can also get gout attacks in your foot, ankle, or knees, or other joints. The attacks can last a few days or many weeks before the pain goes away. Another attack may not happen for months or years.
See your doctor even if your pain from gout is gone. The buildup of uric acid that led to your gout attack can still harm your joints.
How is gout diagnosed?
Your doctor will ask questions about your symptoms and do a physical exam. Your doctor may also take a sample of fluid from your joint to look for uric acid crystals. This is the best way to test for gout. Your doctor may also do a blood test to measure the amount of uric acid in your blood. Your doctor may also do imaging tests, such as ultrasound.
How is it treated?
To stop a gout attack, your doctor can give you a shot of corticosteroids or prescribe a large daily dose of one or more medicines. The doses will get smaller as your symptoms go away. Relief from a gout attack often begins within 24 hours if you start treatment right away.
To ease the pain during a gout attack, rest the joint that hurts. Taking ibuprofen or another anti-inflammatory medicine can also help you feel better. But don’t take aspirin. It can make gout worse by raising the uric acid level in the blood.
To prevent future attacks, your doctor can prescribe a medicine to reduce uric acid buildup in your blood.
Paying attention to what you eat may help you manage your gout. Eat moderate amounts of a healthy mix of foods to control your weight and get the nutrients you need. Limit daily intake of meat, seafood, and alcohol (especially beer). Drink plenty of water and other fluids.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
Cause
Gout is caused by too much uric acid in the blood (hyperuricemia). The exact cause of hyperuricemia sometimes isn’t known, although inherited factors (genes) seem to play a role.
Uric acid may form crystals that build up in the joints. This causes the pain and other symptoms.
Gout can seem to flare up without specific cause. Or it can be brought on by:
- Certain conditions related to diet and body weight, such as being overweight, eating a diet rich in meat and seafood (high-purine foods), and drinking too much alcohol.
- Medicines that may increase uric acid concentration, such as regular use of aspirin or niacin or using medicines that reduce the amount of salt and water in the body (diuretics).
- Major illness or certain medical conditions, such as rapid weight loss or high blood pressure.
- Surgery.
- Having been born with a rare condition that causes high blood uric acid levels. People with Kelley-Seegmiller syndrome or Lesch-Nyhan syndrome have a partial or complete deficiency in an enzyme that helps to control uric acid levels.
Symptoms
Symptoms of gout include:
- Warmth, pain, swelling, and extreme tenderness in a joint, usually a big toe joint. This symptom is called podagra. The pain often starts during the night. It may get worse quickly, last for hours, and be so intense that even light pressure from a sheet is intolerable.
- Very red or purplish skin around the affected joint. The joint may appear to be infected.
- Limited movement in the affected joint.
- Peeling and itching of the skin around the affected joint as the gout gets better.
How symptoms vary
How, where, and when the symptoms of gout appear vary.
- Some people may not experience gout as many painful attacks. Instead they have gout nearly all the time (chronic gout). Chronic gout in older adults may be less painful and can be confused with other forms of arthritis.
- Gout may lead to inflammation of the fluid sacs (bursae) that cushion tissues, particularly in the elbow (olecranon bursitis) and knee (prepatellar bursitis).
- Gout can also affect the joints of the feet, ankles, knees, wrists, fingers, and elbows.
- Symptoms may occur after an illness or surgery.
- Gout may first appear as nodules (tophi) on the hands, elbows, or ears. You may not have any of the classic symptoms of a gout attack.
There are many other conditions with symptoms similar to gout.
What Happens
Gout usually develops after a number of years of buildup of uric acid crystals in the joints and surrounding tissues. A gout attack usually starts during the night with moderate pain that grows worse. A gout attack typically causes pain, swelling, redness, and warmth (inflammation) in a single joint, most often the big toe. Then symptoms gradually go away.
- Most gout attacks stop after about a week.
- Mild attacks may stop after several hours or last for 1 to 2 days. These attacks are often misdiagnosed as tendinitis or a sprain.
- Severe attacks may last up to several weeks, with soreness lasting for up to 1 month.
- Many people have a second attack of gout within 6 months to 2 years after their first attack. But there may be intervals of many years between attacks. If gout is untreated, the frequency of attacks usually increases with time.
There are three stages of gout. Many people never experience the third stage.
- In the first stage, you have high uric acid levels in your blood, but no symptoms. The uric acid levels may stay the same, and you may never have symptoms. Some people may have kidney stones before having their first attack of gout.
- In the second stage, uric acid crystals begin to form, usually in the big toe. You begin to have gout attacks. After an attack, the affected joint feels normal. The time between attacks may grow shorter. Your later attacks may be more severe, last longer, and involve more than one joint.
- In the third stage, symptoms may never go away. They may affect more than one joint. Gritty nodules called tophi may form under your skin.
- Without treatment, the tophi may form in the cartilage of the external ear or the tissues around the joint (bursae, ligaments, and tendons). This can cause pain, swelling, redness, and warmth (inflammation). Progressive crippling and destruction of cartilage and bone is possible.
- This stage of gout is uncommon because of advances in the early treatment of gout.
What Increases Your Risk
Certain things can either cause gout or make you more likely to get it.
Things you can’t change
- Being male
- Having a family history of gout
- Having been born with a rare condition that causes high blood uric acid levels, such as Kelley-Seegmiller syndrome or Lesch-Nyhan syndrome
Medicines that may increase uric acid
- Regular use of aspirin (more than 1 or 2 aspirin a day) or niacin
- Diuretic medicines
- Chemotherapy medicines (usually used to treat cancer)
- Medicines that suppress the immune system, such as cyclosporine, that are used to prevent your body from rejecting an organ transplant
Conditions related to diet and body weight
These include:
- Obesity.
- Moderate, regular, or heavy use of alcohol, especially beer.
- A diet rich in meat and seafood, which can be high in purines.
- Frequent episodes of dehydration.
- Very low-calorie diets.
Other conditions
Certain other conditions and diseases appear more often in people who have gout than in people who don’t, though studies have not shown a clear relationship. Gout may share risk factors (such as obesity, hypertension, and high levels of triglycerides) with certain diseases, including:
- Diabetes.
- Kidney (renal) disease.
- High blood pressure.
- Lead poisoning.
- Hardening of the arteries (atherosclerosis).
- Conditions that cause an abnormal rapid turnover of cells, such as psoriasis, multiple myeloma, hemolytic anemia, or tumors.
- Heart disease.
- Acute illness or infection.
- Injury to a joint.
- Rapid weight loss, as might happen in hospitalized patients who have changes in diet or medicines.
- Surgery.
When should you call your doctor?
Call or see your doctor right away if you have:
- Severe pain in a single joint that comes on very quickly.
- Swollen, tender joints with warm, red skin over them.
It’s important to see your doctor even if the pain from gout has stopped. The uric acid buildup that caused your gout attack may still be irritating your joints and could eventually cause serious damage. Your doctor can prescribe medicines that can prevent and even reverse the uric acid buildup.
Who to see
The following health professionals can diagnose and prescribe treatment for gout:
Exams and Tests
Exams and tests that may help with diagnosis and treatment of gout include:
- A joint fluid analysis (arthrocentesis) to see whether uric acid crystals are present. This is the only certain way to diagnose gout.
- A medical history and physical exam.
- A test to measure levels of uric acid in blood. This may be done if your doctor cannot safely get fluid from the affected joint.
- A test to measure levels of uric acid in urine.
- Imaging tests, such as ultrasound and computed tomography (CT).
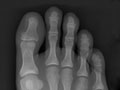
While X-rays of extremities (hands and feet) are sometimes useful in the late stages of the disease, X-rays aren’t usually helpful in the early diagnosis. Pain often causes people to seek medical attention before any long-term changes can be seen on an X-ray. But X-rays may help to rule out other causes of arthritis.
Your doctor may evaluate you for lead poisoning if you have been exposed to lead in your job or through hobbies.
Treatment Overview
The goals of treatment for gout are fast pain relief and prevention of future gout attacks and long-term complications, such as joint destruction and kidney damage. Treatment includes medicines and steps you can take at home to prevent future attacks.
Specific treatment depends on whether you are having an acute attack or are trying to manage long-term gout and prevent future attacks.
To treat an acute attack
- Rest the affected joint(s).
- Use ice to reduce swelling.
- Take short-term medicines at the first sign of a gout attack, as prescribed by your doctor.
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Colchicine
- Corticosteroids
To manage long-term gout and prevent future attacks
If gout symptoms have occurred off and on without treatment for several years, they may become ongoing (chronic) and may affect more than one joint.
- Take medicines as your doctor prescribes for pain.
- Take steps to reduce the risk of future attacks.
- Talk to your doctor about all the medicines you take. Some medicines may raise the uric acid level.
- Manage your weight; get exercise; and limit alcohol, meat, and seafood.
- Take a long-term medicine:
- Uricosuric agents
- Drugs called xanthine oxidase inhibitors
- Colchicine
- Lesinurad
- Pegloticase
- Treat tophi. These are chalky nodules that form from uric acid crystals. Treatment includes:
- Drugs called xanthine oxidase inhibitors, which may shrink the tophi until they disappear.
- In rare cases, surgery to remove large tophi that are causing deformity.
What to think about
If the blood uric acid is high but a person has never had an attack of gout, treatment is rarely needed. But people with extremely elevated levels may need regular testing for signs of kidney damage. And they may need long-term treatment to lower their uric acid levels. Your blood uric acid level may be watched by your doctor until it is lowered to normal levels.
Long-term medicine treatment depends on how high your uric acid levels are and how likely it is that you will have other gout attacks in the future.
After an acute attack of gout, talk with your doctor about the causes of the elevated uric acid levels in your blood. A review of your overall health may reveal diseases, medicines, and habits that could be raising your uric acid levels.
Most doctors will wait several days to weeks after a gout attack is over to begin medicine to lower the high uric acid levels. These medicines can cause uric acid stored elsewhere in the body to begin moving through the bloodstream and could make symptoms worse if treatment begins during a gout attack.
If there is swelling that causes pressure in a large joint such as a knee or ankle, your doctor may relieve the pain and pressure by aspiration. A needle is inserted into the joint and fluid is drawn out (aspirated) with a syringe connected to the needle.
Prevention
Gout usually develops after a number of years of buildup of uric acid crystals in the joints and surrounding tissue. You probably won’t know that you have an elevated uric acid level in your blood until you have had your first gout attack.
But you can help prevent or reduce the severity of future gout attacks. To learn more, see Home Treatment.
Home Treatment
If you have been diagnosed with gout, you can do a lot on your own to treat your condition.
Decrease the pain of an acute attack
- Rest the affected joint until the attack eases and for 24 hours after the attack.
- Elevate painful joints.
- Use ice to reduce swelling.
- Relieve inflammation by taking nonsteroidal anti-inflammatory drugs (NSAIDs). But don’t take aspirin, which may abruptly change uric acid levels and may make symptoms worse. Be safe with medicines. Read and follow all instructions on the label.
- Avoid alcohol, especially beer and hard liquor such as whiskey and gin.
Prevent more attacks
- Control your weight. Being overweight increases your risk for gout. If you are overweight, a diet that is low in fat may help you lose weight. But avoid fasting or very low-calorie diets. Very low-calorie diets increase the amount of uric acid produced by the body and may bring on a gout attack. To learn more, see the topic Weight Management.
- Follow a moderate exercise program.
- Limit alcohol, especially beer. Alcohol can reduce the release of uric acid by the kidneys into your urine, causing an increase of uric acid in your body. Beer, which is rich in purines, appears to be worse than some other beverages that contain alcohol.
- Limit meat and seafood. Diets high in meat and seafood (high-purine foods) can raise uric acid levels.
- Talk to your doctor about all the medicines you take. Some medicines may raise the uric acid level.
- Continue to take the medicines prescribed to you for gout. But if you weren’t taking medicines that lower uric acid (such as allopurinol or probenecid) before the attack, don’t start taking them when the attack begins. These medicines won’t help relieve acute pain. They may actually make it worse.
In the past, gout was thought to be caused by drinking too much alcohol and eating too many rich foods. Although eating certain foods and drinking alcohol may trigger a rise in the level of uric acid in the body, these habits may not by themselves cause gout. Gout is most often caused by an overproduction of uric acid (due to metabolism problems) or decreased elimination of uric acid by the kidneys.
Medications
You use medicine to treat an attack of gout and to reduce the uric acid in the blood. Reducing uric acid helps reduce how often you have attacks.
Medicine choices
Medicine treatment for gout usually involves some combination of short- and long-term medicines.
Short-term medicines
Short-term medicine relieves pain and reduces inflammation during an acute attack or prevents a recurrence of an acute attack. These medicines may include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, indomethacin, or naproxen. Do not take aspirin, which should never be used to relieve pain during a gout attack. Aspirin may change uric acid levels in the blood and may make the attack worse. Be safe with medicines. Read and follow all instructions on the label.
- Colchicine.
- Corticosteroids, which may be given in pills or as a shot for cases of gout that don’t respond to NSAIDs or colchicines.
If treatment is started right away, relief from symptoms often occurs within 24 hours.
During a gout attack, your doctor will prescribe a maximum daily dose of one or more medicines used for short-term treatment to stop the attack. Doses are then reduced as the symptoms go away.
Long-term medicines
Long-term treatment uses medicines to lower uric acid levels in the blood. This can reduce how often you have gout attacks and how severe they are. These medicines may include:
- Uricosuric agents, to increase elimination of uric acid by the kidneys.
- Xanthine oxidase inhibitors, to decrease production of uric acid by the body.
- Colchicine, to prevent flare-ups during the first months that you are taking medicines that lower uric acid.
- Lesinurad. This medicine may be used if xanthine oxidase inhibitors alone have not lowered uric acid levels enough.
- Pegloticase. This medicine is for gout that has lasted a long time and hasn’t responded to other treatment.
If your doctor prescribes medicine to lower your uric acid levels, be sure to take it as directed. Most people will continue to take this medicine every day. It is also important to know how to take it.
- If you’re taking one of these medicines, continue to take the medicine during the attack.
- If you have one of these medicines but have not been taking it, do not start taking the medicine during an attack. Starting these medicines while you are having a gout attack can make your attack much worse.
What to think about
Long-term medicine treatment depends on how high your uric acid levels are and how likely other gout attacks are. In general, the higher your uric acid levels and the more often you have attacks, the more likely it is that long-term medicine treatment will help.
Some people with gout have continuing problems because they don’t take their prescribed medicine. Most people will need treatment every day to keep the uric acid levels in their blood normal. But they may feel perfectly healthy most of the time and wonder why they should keep taking their medicine. If you stop taking your prescribed medicine, nothing may happen at first. But after a while, another gout attack is likely to occur. Without treatment, future attacks are likely to be more severe and occur more often.
Surgery
If gout symptoms have occurred off and on without treatment for more than 10 years, uric acid crystals may have built up in the joints to form gritty, chalky nodules called tophi. If tophi are causing infection, pain, pressure, and deformed joints, your doctor may be able to treat them with medicine. If this doesn’t work, your doctor may recommend surgery to remove them.
Other Treatment
Complementary therapies may be used by some people to relieve symptoms caused by gout.footnote 1
- Cherries and an herb called devil’s claw have been used as anti-inflammatories. Research is needed to evaluate the usefulness of these and other complementary medicines to treat gout.
- Eicosapentaenoic acid (EPA) is known to reduce chronic inflammation. It has not yet been studied to see whether it can help reduce inflammation from gout.
- Although it’s still just a theory, some studies show that folic acid may be helpful in inhibiting the enzyme needed to produce uric acid.
Be sure to talk with your doctor if you are considering taking vitamins, minerals, or other remedies to help reduce future gout attacks.
References
Citations
- Murray MT, Pizzorno JE Jr (2006). Gout. In JE Pizzorno Jr, MT Murray, eds., Textbook of Natural Medicine, 3rd ed., vol. 2, pp. 1703–1709. St. Louis: Churchill Livingstone Elsevier.
Other Works Consulted
- Bhole V, et al. (2010). Epidemiology of gout in women. Arthritis and Rheumatism, 62(4): 1069–1076.
- Burns CM, Wortmann RI (2013). Clinical features and treatment of gout. In GS Firestein et al., eds., Kelley’s Textbook of Rheumatology, 9th ed., vol. 2, pp. 1554–1575. Philadelphia: Saunders.
- Comeau D, et al. (2011). Rheumatology and musculoskeletal problems. In RE Rakel, DP Rakel, eds., Textbook of Family Medicine, 8th ed., pp. 648–689. Philadelphia: Saunders.
- Keenan RT, et al. (2013). Etiology and pathogenesis of hyperuricemia and gout. In GS Firestein et al., eds., Kelley’s Textbook of Rheumatology, 9th ed., vol. 2, pp. 1533–1553. Philadelphia: Saunders.
- Khanna D, et al. (2012). 2012 American College of Rheumatology guidelines for the management of gout. Part 1: Systematic nonpharmacologic and pharmacologic therapeutic approaches to hyperuricemia. Arthritis Care and Research, 64(10): 1431–1446. DOI: 10.1002/acr.21772. Accessed March 11, 2016.
- Khanna D, et al. (2012). 2012 American College of Rheumatology guidelines for the management of gout. Part 2: Therapy and antiinflammatory prophylaxis of acute gouty arthritis. Arthritis Care and Research, 64(10): 1447–1461. DOI: 10.1002/acr.21773. Accessed March 11, 2016.
Current as of: April 1, 2019
Author: Healthwise Staff
Medical Review:Anne C. Poinier, MD – Internal Medicine & E. Gregory Thompson, MD – Internal Medicine & Martin J. Gabica, MD – Family Medicine & Kathleen Romito, MD – Family Medicine & Mary F. McNaughton-Collins, MD, MPH – Internal Medicine
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.