Aortic Valve Regurgitation
Overview
What is aortic valve regurgitation?
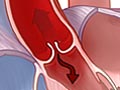
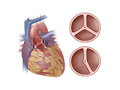
Aortic valve regurgitation is a problem with the aortic valve. The aortic valve allows blood to flow from the heart’s lower left chamber (ventricle) into the aorta and to the body. When the heart rests between beats, the valve closes to keep blood from flowing backward into the heart.
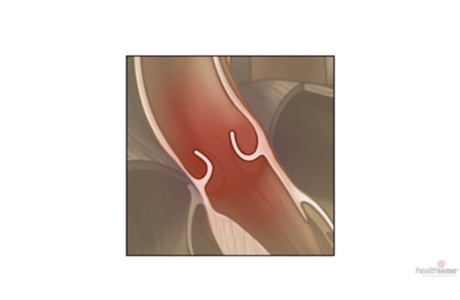
When you have aortic valve regurgitation, the aortic valve doesn’t close as it should. With each heartbeat, some of the blood leaks back (regurgitates) through the aortic valve into the left ventricle. The body does not get enough blood, so the heart has to work harder to make up for it. See a picture of aortic valve regurgitation.
You can have this problem for a long time and not know it. It may take years for symptoms to start. This is called chronicaortic valve regurgitation. In rare cases, the valve problem starts suddenly and without warning. This is called acuteaortic valve regurgitation. It requires medical help right away.
What causes aortic valve regurgitation?
Any condition that damages the aortic valve can cause aortic valve regurgitation. Common causes of chronic valve problems include:
- Being born with a bicuspid aortic valve or a damaged aortic valve.
- Aging.
- Enlargement of the aorta because of high blood pressure or hardening of the arteries.
- Rheumatic fever.
The most common causes of sudden (acute) aortic valve regurgitation include:
- Endocarditis, which is an infection in the heart.
- Aortic dissection, which means that the inner layer of the aorta separates from the middle layer.
- Problems with a replacement (artificial) aortic valve.
- Trauma to the heart valve or aorta.
What are the symptoms?
For chronic regurgitation, you may not have any symptoms at first. But over time you may have:
- Fatigue or weakness.
- Shortness of breath, most often when you are active.
- A fast, slow, or uneven heartbeat (arrhythmia).
- A feeling that your heart is pounding, racing, or beating unevenly (palpitations).
- Chest pain or pressure (angina), often brought on by exercise, when the heart has to work harder.
- Fainting.
If you start to notice any of these symptoms, let your doctor know right away.
When the valve problem is acute, these symptoms are sudden, often more intense, and life-threatening.
How is aortic valve regurgitation diagnosed?
Your doctor may suspect that you have this type of valve problem after hearing a heart murmur through a stethoscope. He or she will ask about your symptoms and past health and will want to know if you have any family history of heart disease.
You will get further tests, like an echocardiogram to confirm the diagnosis, to show how much the valve is leaking, and to see how well the left ventricle is working.
How is it treated?
Your treatment will depend on what is causing your valve problem and if you have symptoms.
If your aortic valve regurgitation starts suddenly and is acute, you’ll need valve replacement surgery right away.
But in most people, aortic valve regurgitation starts slowly. Your doctor will probably recommend some lifestyle changes to keep your heart healthy. He or she may advise you to:
- Quit smoking and stay away from secondhand smoke.
- Follow a heart-healthy diet.
- Be active. Ask your doctor what level and type of exercise is safe for you. You may need to avoid intense activity.
- Stay at a healthy weight, or lose weight if you need to.
Your doctor will see you regularly to check on your heart. In some cases, doctors prescribe medicine to lower blood pressure and delay the advance of the disease.
If regurgitation is severe, if symptoms appear, or if your heart does not pump as well, you will probably need valve replacement surgery.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
Cause
Different factors cause sudden (acute) and long-standing (chronic) aortic valve regurgitation.
Chronic aortic valve regurgitation
Causes of chronic aortic valve regurgitation include:
- Congenital heart defects. Some people are born with a valve that has one (unicuspid valve) or two leaflets (bicuspid valve) instead of three. In either of these cases, the valves don’t close the way they should when the heart is at rest.
- Aging.The normal wear and tear of aging can affect the valves.
- Enlarged aorta. This can be caused by age or other health problems, such as high blood pressure.
- The diet medicine fen-phen. Fen-phen was a popular diet drug that was taken off the U.S. market in 1997 because of its link to heart valve disease, including aortic valve regurgitation.
- Rheumatic fever. If you had rheumatic fever, you may be at increased risk for aortic valve regurgitation.
- Radiation treatments for cancer. In rare cases, radiation treatments to the chest can damage the aortic valve.
Acute aortic valve regurgitation
Acute regurgitation can be caused by:
- Endocarditis. This is an infection in the heart. Bacteria caused by infection can prevent the valve from closing properly.
- Problems with a replacement aortic valve.
- Aortic dissection.
- Trauma to the chest.
Symptoms
Chronic regurgitation
You may not have any symptoms for a long time. When symptoms do appear, it may mean that your heart is severely affected. See a picture of aortic valve regurgitation.
If you start to notice symptoms, let your doctor know right away.
There’s no way to tell how quickly symptoms will develop. Some people stay free of symptoms for decades. For others, symptoms may develop over 2 to 3 years.
Symptoms of aortic valve regurgitation include:
- Shortness of breath, especially with activity.
- Fatigue and weakness.
- Fainting (syncope).
- Trouble breathing at night.
- Swelling in the legs and sometimes the rest of the body (edema).
- Awareness of the heartbeat (palpitations), especially when lying on the left side.
- Dizziness and lightheadedness.
- Abnormal heartbeats (arrhythmias).
- Chest pain or pressure (angina), often brought on by exertion.
Acute regurgitation
These symptoms are sudden, often more intense, and life-threatening. Acute aortic valve regurgitation is an emergency.
What Increases Your Risk
The risk factors for aortic valve regurgitation are:
- Congenital heart defects, such as being born with an aortic valve with one (unicuspid) or two (bicuspid) flaps, called leaflets, rather than three.
- Old age.
- Being male.
- Other health problems, such as Marfan’s syndrome, high blood pressure, and autoimmune diseases.
Tell your doctor if one of your close family members has a congenital aortic valve defect. This may also increase your risk.
When to Call a Doctor
Call your doctor if you have symptoms of aortic valve regurgitation such as fainting, chest pain, or shortness of breath. Your doctor will confirm whether you have valve problems or some other condition. For more information, see Symptoms.
Acute aortic valve regurgitation comes on suddenly. Symptoms include severe shortness of breath, a rapid heart rate, lightheadedness, weakness, confusion, and chest pain.
Acute aortic valve regurgitation is a medical emergency. Call 911 immediately.
Who to see
Health professionals who can diagnose aortic valve regurgitation include:
After you have been diagnosed, you may be referred to a cardiologist, who specializes in heart diseases. The specialist will monitor your condition and help determine when valve replacement is needed.
Exams and Tests
Tests for aortic valve regurgitation can assess how severe the regurgitation is and whether you have any complications, such as abnormal heartbeats (arrhythmias) or heart failure.
Aortic valve regurgitation can typically be diagnosed by physical exam. Your doctor will check your blood pressure, pulse, and listen for abnormal sounds in your heart and lungs.
Other tests may include:
- Echocardiogram (echo). Echocardiography (echo) can be used to look at the heart valves and the shape of the leaflets and to see whether the valves are leaking.
- Electrocardiogram (ECG, EKG). This test checks for a problem with the rhythm of your heartbeat (arrhythmia).
- Magnetic resonance imaging (MRI). This test may be used to check the aortic valve and how well the heart is pumping blood.
- Chest X-ray. This test can show if the lower left ventricle is enlarged.
- Exercise electrocardiogram. This test may be done to see how the heart responds to exercise.
- Cardiac catheterization. This test can help your doctor find out how much the aortic valve is leaking and check the health of your coronary arteries.
- Cardiac pool scan. This test measures how well the left ventricle is pumping and how much blood is pumped out of the chamber with each heartbeat.
|
Severity of aortic valve regurgitation |
How often you should have an echocardiogram |
|---|---|
|
Mild |
Every 3 to 5 years |
|
Moderate |
Every 1 to 2 years |
|
Severe |
At least every 6 to 12 months |
Treatment Overview
Treatment for aortic valve regurgitation usually depends on whether you have symptoms from your leaky heart valve and how well your heart is pumping. Other things that affect treatment include your age and risks related to surgery.
Tests to assess
After your diagnosis, you’ll probably have tests, such as an electrocardiogram or an echocardiogram.
You’ll need regular echocardiogram tests as part of your treatment. Your doctor will let you know how often you’ll get these tests. For more information, see Exams and Tests.
Monitor your symptoms
If you have any chest pain or pressure, fainting, or shortness of breath, be sure to tell your doctor right away. He or she will rely on your report of how you feel and how your symptoms are changing.
Medicines to manage
Medicine cannot treat the leaky heart valve. But you might take medicine to lower blood pressure. If you have an artificial heart valve, you might take medicine to prevent infection or blood clots. For more information, see Medications.
Lifestyle changes
Because your heart is already working hard to keep up with your body’s needs, your doctor will probably recommend that you make some healthy lifestyle changes. These include eating a heart-healthy diet and not smoking. For more information, see Living With Aortic Regurgitation.
Surgery if you get worse
You might have surgery to replace your aortic valve if your regurgitation is getting worse. You might have surgery before you get symptoms. If you have acute regurgitation, surgery may be done right away. For more information, see Surgery.
End-of-life care
You may want to consider the type of care you wish to receive in case you are unable to make your wishes known. For more information, see the topic Care at the End of Life.
Living With Aortic Regurgitation
Having aortic valve regurgitation means that your heart is working overtime to keep up with your body’s needs. Your doctor will probably suggest lifestyle changes to help your heart.
Make healthy lifestyle changes
- If you smoke, try to quit. Medicines and counseling can help you quit for good.
- Your doctor will also recommend that you follow a heart-healthy diet and limit how much sodium you eat.
- If you don’t have symptoms of aortic valve regurgitation and your left ventricle is working well, your doctor may suggest regular, light aerobic exercise, such as walking. But don’t start an exercise program on your own without first talking with your doctor. You may need some tests to see what sort of exercise is safe for you.
- If you need to lose weight, try to reach and stay at a healthy weight. For help, see the topic Weight Management.
Take care of yourself
- See your doctor right away if you have new symptoms or symptoms that get worse. Symptoms may include chest pain or pressure, fainting, and shortness of breath. These are signs that you are likely to need surgery.
- If your aortic valve regurgitation is severe, your doctor will probably advise you to avoid strenuous physical activity.
- See your doctor regularly, and get the tests you need to assess your heart, such as echocardiograms. For more information, see Exams and Tests.
- Manage other health problems including high blood pressure, diabetes, and high cholesterol.
- Practice good dental hygiene and have regular checkups. Good dental health is especially important, because bacteria can spread from infected teeth and gums to the heart valves.
- Get a flu vaccine every year. Get a pneumococcal vaccine shot. If you have had one before, ask your doctor if you need another dose.
- Talk with your doctor if you have concerns about sex and your heart. Your doctor can help you know if or when it’s okay for you to have sex.
Medications
Treatment for chronic aortic valve regurgitation includes medicines to reduce blood pressure. If you have valve replacement surgery, you may need to take medicines to prevent infection and blood clots around the artificial valve.
Medicines to reduce blood pressure
- Angiotensin II receptor blockers (ARB)
- Angiotensin-converting enzyme (ACE) inhibitors
- Beta-blockers
- Calcium channel blockers
Medicines for other problems
- Medicines to treat atrial fibrillation.
- Digoxin and diuretics help relieve symptoms of heart failure.
- Nitrates (such as nitroglycerin) relieve angina symptoms, such as chest pain or pressure.
Medicines after valve surgery
If you have valve replacement surgery, you may need:
- Anticoagulants. You may take an anticoagulant, also called a blood thinner, to prevent blood clots, especially if you had surgery to replace your aortic valve.
- Antibiotics before you have certain dental or surgical procedures. The antibiotics help prevent an infection in your heart called endocarditis.
Surgery
Valve replacement surgery can fix aortic valve regurgitation. Surgery to repair the aortic valve, instead of replacing it, is not commonly done. Having surgery is a big decision. To help decide when you need surgery, you and your doctor will look at your overall health, your heart health, and how severe your regurgitation is.
Your doctor will check:
- Your symptoms, if you have any.
- Your ejection fraction (how much blood your heart is pumping out to your body).
- The size of your left ventricle.
If you need some other heart surgery, such as bypass surgery, your doctor may suggest valve replacement at the same time.
Even if you don’t have symptoms, your doctor may suggest surgery. Most of the time, symptoms only occur when the heart is already damaged. Learn more about deciding about surgery for aortic valve replacement.
If you have surgery, a mechanical or tissue valve will be used to replace your heart valve. Before you have surgery, you and your doctor will decide on which type of valve is right for you. To help with this decision, see:
References
Citations
- Nishimura RA, et al. (2014). 2014 AHA/ACC guideline for the management of patients with valvular heart disease: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation, published online March 3, 2014. DOI: 10.1161/CIR.0000000000000031. Accessed May 1, 2014.
Other Works Consulted
- Freeman RV, Otto CM (2011). Aortic valve disease. In V Fuster et al., eds., Hurst’s The Heart, 13th ed., vol. 2, pp. 1692–1720. New York: McGraw-Hill.
- Nishimura RA, et al. (2014). 2014 AHA/ACC guideline for the management of patients with valvular heart disease: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation, published online March 3, 2014. DOI: 10.1161/CIR.0000000000000031. Accessed May 1, 2014.
- Oakley RE, et al. (2008). Choice of prosthetic heart valve in today’s practice. Circulation, 117(2): 253–256.
- Otto CM, Bonow RO (2012). Valvular heart disease. In RO Bonow et al., eds., Braunwald’s Heart Disease: A Textbook of Cardiovascular Medicine, 9th ed., vol. 2, pp. 1468–1539. Philadelphia: Saunders.
- Rosengart TK, et al. (2008). Percutaneous and minimally invasive valve procedures: A scientific statement from the American Heart Association Council on Cardiovascular Surgery and Anesthesia, Council on Clinical Cardiology, Functional Genomics and Translational Biology Interdisciplinary Working Group, and Quality of Care and Outcomes Research Interdisciplinary Working Group. Circulation, 117(13): 1750–1767.
- Stewart WJ, Carabello BA (2007). Aortic valve disease. In EJ Topol et al., eds., Textbook of Cardiovascular Medicine, 3rd ed., pp. 366–388. Philadelphia: Lippincott Williams and Wilkins.
- Stout KK, Verrier ED (2009). Acute valvular regurgitation. Circulation, 119(25): 3232–3241.
- Whitlock RP, et al. (2012). Antithrombotic and thrombolytic therapy for valvular disease: Antithrombotic therapy and prevention of thrombosis, 9th ed.—American College of Chest Physicians evidence-based clinical practice guidelines. Chest, 141(2, Suppl): e576S–e600S.
Current as of: April 9, 2019
Author: Healthwise Staff
Medical Review:Rakesh K. Pai, MD – Cardiology, Electrophysiology & Martin J. Gabica, MD – Family Medicine & E. Gregory Thompson, MD – Internal Medicine & Adam Husney, MD – Family Medicine & Michael P. Pignone, MD, MPH, FACP – Internal Medicine
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.