Parkinson’s Disease
Topic Overview
What is Parkinson’s disease?
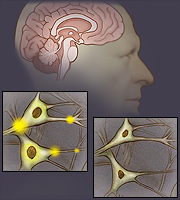
Parkinson’s disease affects the way you move. It happens when there is a problem with certain nerve cells in the brain.
Normally, these nerve cells make an important chemical called dopamine. Dopamine sends signals to the part of your brain that controls movement. It lets your muscles move smoothly and do what you want them to do. When you have Parkinson’s, these nerve cells break down. Then you no longer have enough dopamine, and you have trouble moving the way you want to.
Parkinson’s is progressive, which means it gets worse over time. But usually this happens slowly, over many years. And there are good treatments that can help you live a full life.
What causes Parkinson’s disease?
No one knows for sure what makes these nerve cells break down. But scientists are doing a lot of research to look for the answer. They are studying many possible causes, including aging and poisons in the environment.
Abnormal genes seem to lead to Parkinson’s disease in some people. But so far, there is not enough proof to show that it is always inherited.
What are the symptoms?
The four main symptoms of Parkinson’s are:
- Tremor, which means shaking or trembling. Tremor may affect your hands, arms, or legs.
- Stiff muscles.
- Slow movement.
- Problems with balance or walking.
Tremor may be the first symptom you notice. It’s one of the most common signs of the disease, although not everyone has it.
More importantly, not everyone with a tremor has Parkinson’s disease.
Tremor often starts in just one arm or leg or on only one side of the body. It may be worse when you are awake but not moving the affected arm or leg. It may get better when you move the limb or you are asleep.
In time, Parkinson’s affects muscles all through your body, so it can lead to problems like trouble swallowing or constipation.
In the later stages of the disease, a person with Parkinson’s may have a fixed or blank expression, trouble speaking, and other problems. Some people also lose mental skills (dementia).
People usually start to have symptoms between the ages of 50 and 60. But sometimes symptoms start earlier.
How is Parkinson’s disease diagnosed?
Your doctor will ask questions about your symptoms and your past health and will do a neurological exam. This exam includes questions and tests that show how well your nerves are working. For example, your doctor will watch how you move, check your muscle strength and reflexes, and check your vision.
Your doctor will also ask questions about your mood.
In some cases, your doctor may have you try a medicine. How this medicine works may help your doctor know if you have Parkinson’s disease.
There are no lab or blood tests that can help your doctor know whether you have Parkinson’s. But you may have tests to help your doctor rule out other diseases that could be causing your symptoms. For example, you might have an MRI to look for signs of a stroke or brain tumor.
How is it treated?
At this time, there is no cure for Parkinson’s disease. But there are several types of medicines that can control the symptoms and make the disease easier to live with.
You may not even need treatment if your symptoms are mild. Your doctor may wait to prescribe medicines until your symptoms start to get in the way of your daily life. Your doctor will adjust your medicines as your symptoms get worse. You may need to take several medicines to get the best results.
Levodopa (also called L-dopa) is the best drug for controlling symptoms of Parkinson’s. But it can cause problems if you use it for a long time or at a high dose. So doctors sometimes use other medicines to treat people in the early stages of the disease.
The decision to start taking medicine, and which medicine to take, will be different for each person. Your doctor will be able to help you make these choices.
In some cases, a treatment called deep brain stimulation may also be used. For this treatment, a surgeon places wires in your brain. The wires carry tiny electrical signals to the parts of the brain that control movement. These little signals can help those parts of the brain work better.
There are many things you can do at home that can help you stay as independent and healthy as possible. Eat healthy foods. Get the rest you need. Make wise use of your energy. Get some exercise every day. Physical therapy and occupational therapy can also help.
How will Parkinson’s disease affect your life?
Finding out that you have a long-term, progressive disease can lead to a wide range of feelings. You may feel angry, afraid, sad, or worried about what lies ahead. It may help to keep a few things in mind:
- Usually this disease progresses slowly. Some people live for many years with only minor symptoms.
- Many people are able to keep working for years. As the disease gets worse, you may need to change how you work.
- It is important to take an active role in your health care. Find a doctor you trust and can work with.
- Depression is common in people who have Parkinson’s. If you feel very sad or hopeless, talk to your doctor or see a counselor.
- It can make a big difference to know that you’re not alone. Ask your doctor about Parkinson’s support groups, or look for online groups or message boards.
- Parkinson’s affects more than just the person who has it. It also affects your loved ones. Be sure to include them in your decisions.
Cause
Low levels of dopamine, a brain chemical involved in controlling movement, cause symptoms of Parkinson’s disease. Low levels happen when nerve cells in a part of the brain that makes dopamine break down. The exact cause of this breakdown isn’t known.
Scientists are looking for links between Parkinson’s disease and genetics, aging, toxins in the environment, and free radicals. Although these studies are beginning to provide some answers, experts don’t know the exact cause of the disease.
Only a small percentage of people with Parkinson’s have a parent, brother, or sister who has the disease. But abnormal genes do seem to be a factor in a few families where early-onset Parkinson’s is common.
There are many other causes of parkinsonism, which is a group of symptoms that includes tremor, muscle stiffness, slow movement, and unsteady walking. Parkinsonism mimics Parkinson’s disease, but in fact is not Parkinson’s disease.
Symptoms
Symptoms of Parkinson’s disease differ from person to person. They also change as the disease progresses. Symptoms that one person gets in the early stages of the disease, another person may not get until later—or not at all.
Symptoms typically begin appearing between the ages of 50 and 60. They develop slowly and often go unnoticed by family, friends, and even the person who has them.
The disease causes motor symptoms and non-motor symptoms. Motor symptoms are those that have to do with how you move. The most common one is tremor.
Tremor
Tremor, or shaking, often in a hand, arm, or leg, occurs when you’re awake and sitting or standing still (resting tremor), and it gets better when you move that body part.
Tremor is often the first symptom that people with Parkinson’s disease or their family members notice.
At first the tremor may appear in just one arm or leg or only on one side of the body. The tremor also may affect the chin, lips, and tongue.
As the disease progresses, the tremor may spread to both sides of the body. But in some cases the tremor remains on just one side.
Emotional and physical stress tends to make the tremor more noticeable. Sleep, complete relaxation, and intentional movement or action usually reduce or stop the tremor.
Although tremor is one of the most common signs of Parkinson’s, not everyone with tremor has Parkinson’s. Unlike tremor caused by Parkinson’s, tremor caused by other conditions gets better when your arm or hand is not moving and gets worse when you try to move it.
The most common cause of non-Parkinson’s tremor is essential tremor. It’s a treatable condition that is often wrongly diagnosed as Parkinson’s.
Other common symptoms
Besides tremor, the most common symptoms include:
- Stiff muscles (rigidity) and aching muscles.One of the most common early signs of Parkinson’s is a reduced arm swing on one side when you walk. This is caused by rigid muscles. Rigidity can also affect the muscles of the legs, face, neck, or other parts of the body. It may cause muscles to feel tired and achy.
- Slow, limited movement, especially when you try to move from a resting position. For instance, it may be hard to get out of a chair or turn over in bed.
- Weakness of face and throat muscles. It may get harder to talk and swallow. You may choke, cough, or drool. Speech becomes softer and monotonous. Loss of movement in the muscles in the face can cause a fixed, vacant facial expression, often called the “Parkinson’s mask.”
- Difficulty with walking and balance. A person with this disease is likely to take small steps and shuffle with his or her feet close together, bend forward slightly at the waist, and have trouble turning around. Balance and posture problems may cause frequent falls. But these problems usually don’t happen until later on.
- Freezing, a sudden, brief inability to move. It most often affects walking.
A small number of people have symptoms on only one side of the body that never move to the other side.
Non-motor symptoms
Parkinson’s disease can cause many other symptoms that aren’t related to how you move. These can be disabling and may include things like constipation, sleep problems, and depression.
There are many other conditions with symptoms similar to Parkinson’s disease. Some of these may be reversible.
What Happens
Treatment may help control symptoms during the early stages of Parkinson’s disease. It is usually started as soon as symptoms begin to affect your ability to work or do daily activities. As the disease progresses, drugs may become less effective.
Early stage
Tremor is usually the first symptom, appearing in just one arm or leg or on only one side of the body. With time, the tremor usually—but not always—spreads to both sides of the body. Joint pain, weakness, and fatigue may occur.
Moderate stage
As the disease gets worse, the person may have slow movement, stiff muscles, and poor coordination. He or she may have problems with tasks such as writing, shaving, or brushing teeth. Changes in handwriting are common.
Problems with posture and balance develop. A person with Parkinson’s tends to walk in a stooped manner with quick, shuffling steps.
Advanced stage
After several years, as muscle stiffness and tremor increase, the person may become unable to care for himself or herself. He or she may be confined to a wheelchair or bed.
People who have taken medicine for several years may not only notice their symptoms getting worse but also may start to have other movement problems. These motor fluctuations can be reduced somewhat by making changes in the person’s medicine, but they can be difficult to control and may further complicate treatment.
Dementia may develop in up to one-third of people who have late-stage Parkinson’s disease.footnote 1 Dementia symptoms may include disorientation at night, confusion, and memory loss. Treatment for Parkinson’s disease can also contribute to this problem.
What Increases Your Risk
A risk factor is anything that increases your chances of getting sick or having a problem. Risk factors for Parkinson’s disease are hard to identify, because the cause of the disease is unknown.
Getting older
Advancing age is the only known risk factor for typical Parkinson’s disease (not including early-onset Parkinson’s). Most instances of Parkinson’s occur after age 50. But the illness does occur in people between the ages of 30 and 50 or, in rare cases, at a younger age.
Family history
A very small number of people with Parkinson’s have a close relative who also has the disease. But it doesn’t appear that a family history of typical Parkinson’s significantly increases your risk for the disease.
Having a family history of the disease is a more significant risk factor in cases of early-onset Parkinson’s, but this form of the disease is not common.
Poisons in the environment
Some research suggests that long-term exposure to certain environmental risk factors such as pesticides, chemicals, or well water may increase a person’s risk of developing Parkinson’s disease.
When should you call your doctor?
If you develop a tremor
Urgent medical care isn’t needed if you have had a tremor—shaking or trembling—for some time. But you should discuss the tremor at your next doctor’s appointment.
If a tremor is affecting your daily activities or if it is a new symptom, see your doctor sooner.
A written description will help your doctor make a correct diagnosis. In writing your description, consider the following questions:
- Did the tremor start suddenly or gradually?
- What makes it worse or better?
- What parts of your body are affected?
- Have there been any recent changes in the medicines you are taking or how much you are taking?
If you have Parkinson’s disease
If you have been diagnosed with Parkinson’s, call your doctor if:
- You notice any significant change in your symptoms, such as severe episodes of freezing—a sudden loss of mobility—which may affect walking.
- Your response to your medicine changes.
- Any other symptoms occur, such as constipation, sexual problems, or incontinence.
- You have symptoms of depression, such as feeling sad or losing interest in daily activities.
- You or your family notice that you have problems with memory and thinking ability.
Who to see
The following health professionals can help diagnose or treat Parkinson’s disease:
Other health professionals who may be involved in your care include the following:
Exams and Tests
A diagnosis of Parkinson’s disease is based on your medical history and a thorough neurological exam.
Your doctor also may check your sense of smell.
In some cases, your doctor will have you try a medicine for Parkinson’s disease. If that medicine helps your symptoms, it may help the doctor find out if you have the disease.
Tests
There are no lab tests that can diagnose Parkinson’s.
But if your doctor isn’t sure you have Parkinson’s, he or she may do certain tests to see if you have another condition with similar symptoms.
For instance, blood tests may be done to check for abnormal thyroid hormone levels or liver damage. An imaging test (such as a CT scan or an MRI) may be used to check for signs of a stroke or brain tumor.
Another type of imaging test, called PET, sometimes may detect low levels of dopamine in the brain, a key feature of Parkinson’s. But PET scanning isn’t commonly used to evaluate Parkinson’s because it’s very expensive, not available in many hospitals, and only used experimentally.
Treatment Overview
No known treatment can stop or reverse the breakdown of nerve cells that causes Parkinson’s disease. But there are many treatments that can help your symptoms and improve your quality of life.
Your age, work status, family, and living situation can all affect decisions about when to begin treatment, what types of treatment to use, and when to make changes in treatment. As your medical condition changes, you may need regular changes in your treatment to balance quality-of-life issues, side effects of treatment, and treatment costs.
You’ll need to see members of your health care team regularly (every 3 to 6 months, or as directed) for adjustments in your treatment as your condition changes.
Treatments for Parkinson’s include:
- Medicines, such as levodopa and dopamine agonists. This is the most common treatment for Parkinson’s disease. For more information, see Medications.
- Home treatment. There are many steps you can take at home to make dealing with the symptoms of Parkinson’s disease easier, such as getting regular exercise and eating a healthy diet. For more information, see Home Treatment.
- Surgery. Brain surgery, for example deep brain stimulation (DBS), may be considered when medicine fails to control symptoms of Parkinson’s disease or causes severe or disabling side effects. For more information, see Surgery.
- Speech therapy. Speech therapists use breathing and speech exercises to help you overcome the soft, imprecise speech and monotone voice that develop in advanced Parkinson’s disease.
- Physical therapy. Therapists may help you improve your walking and reduce your risk of falling.
- Occupational therapy. Therapists can help you learn new ways to do things for yourself so you can stay independent longer.
- Treatment for mental problems. You or your family members may notice that you begin to have problems with memory, problem solving, learning, and other mental functions. When these problems keep you from doing daily activities, it is called dementia. There are medicines that can help treat dementia in people with Parkinson’s.
Depression
Depression is common in people with Parkinson’s disease. Recognizing and dealing with depression is important. There are medicines that can help the symptoms of depression in people with Parkinson’s.
Your doctor, other health professionals, or Parkinson’s support groups can help you get emotional support and education about the illness. This is important both early and throughout the course of the disease.
Palliative care
Palliative care is a kind of care for people who have a serious illness. It’s different from care to cure your illness. Its goal is to improve your quality of life—not just in your body but also in your mind and spirit.
You can have this care along with treatment to cure your illness. You can also have it if treatment to cure your illness no longer seems like a good choice.
Palliative care providers will work to help control pain or side effects. They may help you decide what treatment you want or don’t want. And they can help your loved ones understand how to support you.
If you’re interested in palliative care, talk to your doctor.
For more information, see the topic Palliative Care.
Prevention
There is no known way to prevent Parkinson’s disease.
Some studies have tried to find a link between the Mediterranean-style diet and a lower risk of diseases such as Parkinson’s disease. More research is needed.
Home Treatment
Early on, Parkinson’s disease may not greatly disrupt your life. But for most people, the disease becomes more disabling over time. Home treatment can help you adjust as time goes on and help you stay independent for as long as possible.
Your home and lifestyle
- Modify your activities and your home. For example, simplify your daily activities, and change the location of furniture so that you can hold on to something as you move around the house.
- Eat healthy foods, including plenty of fruits, vegetables, grains, cereals, legumes, poultry, fish, lean meats, and low-fat dairy products.
- Exercise and do physical therapy. They have benefits in both early and advanced stages of the disease.
Motor problems
- Deal with tremor. This may include putting a little weight on your hand to help reduce tremor and restore control.
- Improve speech quality by working with a speech therapist (also called a speech-language pathologist).
- Reduce problems with eating and drooling by changing how and what you eat.
- Deal with “freezing” by various means, such as stepping toward a specific target on the ground.
- Deal with sexual function problems. Talk to your doctor about your specific issues. He or she may be able to suggest a change in your treatment, such as a change in your medicine or exercise.
Mood and mental problems
- Deal with depression. If you are feeling sad or depressed, ask a friend or family member for help. If these feelings don’t go away, or if they get worse, talk to your doctor. He or she may be able to suggest someone for you to talk to. Or your doctor may give you medicine that will help.
- Deal with dementia. Dementia is common late in Parkinson’s disease. Symptoms may include confusion and memory loss. If you (or a family member) notice that you are confused a lot or have trouble thinking clearly, talk to your doctor. There are medicines that can help dementia in people with Parkinson’s disease.
Medications
Medicines are the most common treatment for Parkinson’s disease. The goal is to correct the shortage of the brain chemical dopamine, which causes the symptoms of Parkinson’s.
The decision to start taking medicine, and which medicine to take, will be different for each person. Medicine is usually started when your symptoms become disabling or disrupt your daily activities.
Symptoms change as the disease progresses. Because of this, your doctor will adjust your medicine to deal with the symptoms as they appear.
Medicines often improve symptoms, but they also may cause side effects. It may take some time to find the best combination of medicines for you.
Medication choices
Several medicines may be used at different stages of the disease:
- Levodopa and carbidopa
- Dopamine agonists (for example, pramipexole or ropinirole)
- COMT inhibitors (entacapone, tolcapone)
- MAO-B inhibitors (rasagiline, selegiline)
- Amantadine
- Anticholinergic agents (for example, benztropine or trihexyphenidyl)
- Apomorphine
Levodopa is thought to be the most effective drug for controlling symptoms. But many doctors prescribe dopamine agonists in the beginning of the disease. This is because after a few years, levodopa can cause motor complications (times when the medicine suddenly stops working or when you have uncontrollable jerking movements). Talk to your doctor about which medicines are best for you.
Although it’s always important to follow your doctor’s instructions when you take medicines, it’s especially vital when you have Parkinson’s.
Increasing, decreasing, or stopping the medicines you are taking may cause big changes in your symptoms and can be dangerous. Even if a medicine doesn’t seem to be working, when you stop taking it, your symptoms of Parkinson’s disease may be worse.
Taking medicine with food
Early in the disease, it might be helpful to take pills with food to help with nausea, which may be caused by some of the medicines for Parkinson’s disease.
Later in the disease, taking the medicines at least 1 hour before meals (and at least 2 hours after meals) may help them work best.
Some medicines for Parkinson’s disease don’t work as well if you take them at the same time you eat food with protein in it, such as meat or cheese. The protein can block the medicine and keep it from working as well as it should.
Surgery
Brain surgery may be considered when drugs fail to control symptoms of Parkinson’s disease or cause severe or disabling side effects.
Surgery isn’t a cure. Drugs are usually still needed after surgery. But you probably won’t need as much medicine as before, which means you may have fewer side effects.
People who have very advanced Parkinson’s or who have other serious problems (such as heart or lung disease, cancer, or kidney failure) usually aren’t good candidates for surgery. Surgery usually isn’t considered for people who have dementia or psychiatric disorders.
Surgery choices
- Deep brain stimulation uses electrical impulses to stimulate a target area in the brain. It’s the preferred surgery for treating most cases of advanced Parkinson’s.
- Pallidotomy involves the precise destruction of a very small area in a deep part of the brain that causes symptoms.
- Thalamotomy involves the precise destruction of a very small area in another part of the brain that causes symptoms.
Neurotransplantation is an experimental procedure being studied for the treatment of Parkinson’s disease. It involves implanting cells that produce dopamine into the brain. Information about how well neurotransplantation works is limited. And it is not a proven treatment or a realistic option for most people at this time.
See a neurologist
A neurologist with special training in Parkinson’s disease is most often the best kind of doctor to make a decision about surgery. If you might benefit from surgery or deep brain stimulation, your neurologist can refer you to a brain surgeon with experience doing these operations.
Other Treatment
Physical therapy, speech and language therapy, and occupational therapy can all be helpful for people who have Parkinson’s disease.
Special diets
Several nutritional therapies have been suggested as treatments for Parkinson’s. None of these have been proved effective. But it is important to maintain general health and to eat a balanced diet.
Before trying a complementary treatment, such as a special diet, talk with your doctor about the safety and potential side effects of the treatment. Talking with your doctor can help you both decide whether a treatment is safe and effective. Complementary treatments should not replace the use of medicines to treat Parkinson’s if you are a candidate for treatment with these medicines.
Electroconvulsive therapy
Depression that does not respond to drugs may improve with electroconvulsive therapy (ECT). ECT can also improve movement for a short period of time, though the reason for this improvement isn’t understood.
Current as of: March 28, 2019
Author: Healthwise Staff
Medical Review:Anne C. Poinier, MD – Internal Medicine & Martin J. Gabica, MD – Family Medicine & Elizabeth T. Russo, MD – Internal Medicine & Kathleen Romito, MD – Family Medicine & G. Frederick Wooten Jr., MD – Neurology
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.

