Pericarditis
Topic Overview
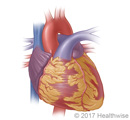
What is pericarditis?
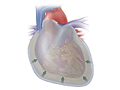
Pericarditis is swelling and irritation of the pericardium, which is the sac that surrounds your heart.
Pericarditis usually doesn’t cause serious problems. Most people get better in 7 to 10 days. When there are problems, they may include:
- A buildup of fluid in the pericardial sac (pericardial effusion).
- Sudden pressure on the heart and sudden difficulty pumping enough blood (called cardiac tamponade). This can be caused by the weight and pressure of the fluid buildup if it happens quickly.
- Constrictive pericarditis, in which the sac around the heart gets thick and stiff. This makes it harder for the heart to pump blood.
What causes pericarditis?
Many things can cause pericarditis, including:
- Viral infection. This is the most common cause.
- Heart attack.
- Chest injury.
- Recent heart surgery.
- Certain diseases, such as cancer, lupus, or tuberculosis.
In many cases, the cause is not known.
What are the symptoms?
The main symptom is a sharp pain in the center or left side of your chest. The pain may spread to the shoulder blade. For some people, this pain is dull instead of sharp. It may be worse when you lie down or take a deep breath.
The pain lasts for hours or days and doesn’t get better when you rest. It’s different from a type of chest pain called angina, which only lasts a short time and usually gets better with rest.
Other symptoms may include a mild fever, weakness, and feeling very tired.
Pericarditis usually isn’t dangerous. But your chest pain could be caused by something more serious, like a heart attack. Getting diagnosed and treated early can help keep pericarditis from leading to other problems. That’s why you should call a doctor right away if you have any kind of sudden chest pain.
How is pericarditis diagnosed?
Your doctor will listen to your heart during a physical exam. He or she will also ask questions about your medical history, such as whether you’ve had a recent illness, radiation treatment for cancer, or tuberculosis.
Your doctor may want you to have some tests, including an echocardiogram, electrocardiogram, chest X-ray, and blood tests.
How is it treated?
If there are no other problems, pericarditis usually goes away on its own in a couple of weeks. During this time:
- Your doctor may prescribe a medicine to relieve pain and reduce swelling. Medicines may include a nonsteroidal anti-inflammatory drug (NSAID), such as aspirin or ibuprofen, or another type of medicine called colchicine. Be safe with medicines. Read and follow all instructions on the label.
- Get plenty of rest. Avoid exercise and strenuous activity. Ask your doctor when you can be active again.
- Follow your doctor’s advice about what problems to watch for, such as shortness of breath or other signs of complications.
Be sure to keep all follow-up appointments with your doctor. If you have complications or the illness gets worse, you may need further treatment. This could include medicines or a procedure to relieve the fluid and pressure around your heart (pericardiocentesis).
References
Other Works Consulted
- Adler Y, et al. (2015). ESC Guidelines for the diagnosis and management of pericardial diseases. European Heart Journal, 36(42): 2921–2964. DOI: doi/10.1093/eurheartj/ehv318. Accessed April 22, 2016.
- Hoit BD (2011). Pericardial disease. In V Fuster et al., eds., Hurst’s the Heart, 13th ed., vol. 2, pp. 1917–1939. New York: McGraw-Hill.
- LeWinter MM, Hopkins WE (2015). Pericardial diseases. In DL Mann et al., eds., Braunwald’s Heart Disease: A Textbook of Cardiovascular Medicine, 10th ed., vol. 2, pp. 1636–1657. Philadelphia: Saunders.
Credits
Current as ofApril 9, 2019
Author: Healthwise Staff
Medical Review: Rakesh K. Pai, MD – Cardiology, Electrophysiology
E. Gregory Thompson, MD – Internal Medicine
Martin J. Gabica, MD – Family Medicine
Kathleen Romito, MD – Family Medicine
Adam Husney, MD – Family Medicine
Stephen Fort, MD, MRCP, FRCPC – Interventional Cardiology
Current as of: April 9, 2019
Author: Healthwise Staff
Medical Review:Rakesh K. Pai, MD – Cardiology, Electrophysiology & E. Gregory Thompson, MD – Internal Medicine & Martin J. Gabica, MD – Family Medicine & Kathleen Romito, MD – Family Medicine & Adam Husney, MD – Family Medicine & Stephen Fort, MD, MRCP, FRCPC – Interventional Cardiology
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.