High Blood Pressure
Topic Overview
What is high blood pressure?
It’s normal for blood pressure to go up and down throughout the day. But if it stays up, you have high blood pressure. Another name for high blood pressure is hypertension.
High blood pressure increases the risk of stroke, heart attack, and other problems. You and your doctor will talk about your risks of these problems based on your blood pressure.
Your doctor will give you a goal for your blood pressure. Your goal will be based on your health and your age.
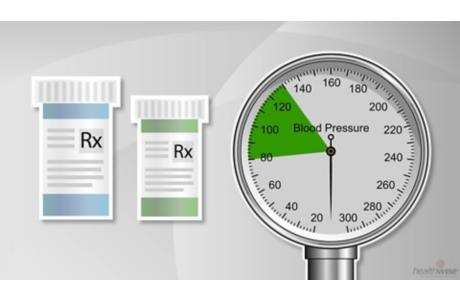
Your blood pressure consists of two numbers: systolic and diastolic. Someone with a systolic pressure of 120 and a diastolic pressure of 80 has a blood pressure of 120/80, or “120 over 80.” Blood pressure is measured in millimeters of mercury (mm Hg).
- The systolic number shows how hard the blood pushes when the heart is pumping.
- The diastolic number shows how hard the blood pushes between heartbeats, when the heart is relaxed and filling with blood.
What causes high blood pressure?
In most cases, doctors can’t point to the exact cause. But several things are known to raise blood pressure, including being very overweight, drinking too much alcohol, having a family history of high blood pressure, eating too much salt, and getting older.
Your blood pressure may also rise if you are not very active, you don’t eat enough potassium and calcium, or you have a condition called insulin resistance.
What are the symptoms?
High blood pressure doesn’t usually cause symptoms. Most people don’t know they have it until they go to the doctor for some other reason.
Very high blood pressure can cause severe headaches and vision problems. These symptoms can also be caused by dangerously high blood pressure called hypertensive emergency. It may also be called a hypertensive crisis or malignant high blood pressure. It’s a medical emergency.
How is high blood pressure diagnosed?
Most people find out that they have high blood pressure during a routine doctor visit. After measuring your blood pressure, your doctor may ask you to test it again when you are home.footnote 1, footnote 3
How is it treated?
If you have high blood pressure, your doctor will give you a blood pressure goal. Your goal will be based on your health and your age.
You can help lower your blood pressure by making healthy changes in your lifestyle. If those lifestyle changes don’t work well enough, you may also need to take pills. Either way, you will need to control your high blood pressure throughout your life.
Treatment depends on how high your blood pressure is, whether you have other health problems such as diabetes, and whether any organs have already been damaged. Your doctor may also check your risk for other problems, such as heart attack and stroke.
Most people take more than one pill for high blood pressure. Work with your doctor to find the right pill or combination of pills that will cause the fewest side effects.
What can you do to prevent high blood pressure?
Making lifestyle changes can help you to prevent high blood pressure. You can:
- Stay at a healthy weight or lose extra weight.
- Eat heart-healthy foods and limit sodium.
- Exercise regularly.
- Limit alcohol to 2 drinks a day for men and 1 drink a day for women.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
- Fitness: Adding More Activity to Your Life
- Healthy Eating: Eating Less Sodium
- Healthy Eating: Starting a Plan for Change
- High Blood Pressure: Checking Your Blood Pressure at Home
- High Blood Pressure: Taking Medicines Properly
- High Blood Pressure: Using the DASH Diet
- Low-Salt Diets: Eating Out
- Quitting Smoking: Coping With Cravings and Withdrawal
- Quitting Smoking: Getting Support
- Stress Management: Doing Meditation
- Stress Management: Doing Progressive Muscle Relaxation
- Weight Management: Stop Negative Thoughts
Cause
Experts know that many things are linked to high blood pressure. But experts still don’t fully understand the exact cause. Things that are linked to high blood pressure include:
- Aging.
- Drinking more than 2 alcoholic drinks a day for men or more than 1 alcoholic drink a day for women.
- Eating a lot of sodium (salt).
- Being overweight or obese.
- Not exercising.
- Being under a lot of stress.
- Eating a diet low in potassium, magnesium, and calcium.
Primary, or essential, high blood pressure is the most common type of high blood pressure. Most people who have high blood pressure have primary high blood pressure.
Secondary high blood pressure, which is caused by another disease or medicine, is less common.
Elevated blood pressure readings may not always mean that you have high blood pressure. For some people, just being in a medical setting causes their blood pressure to rise. This is called white-coat hypertension.
Symptoms
People who have high blood pressure usually don’t have any symptoms. Most people who have high blood pressure feel fine. It’s during a routine exam or a doctor visit for another problem that they find out that they have high blood pressure.
Very severe high blood pressure (such as 180 over 120 or higher) may lead to hypertensive emergency. This is also called malignant hypertension. A hypertensive emergency needs immediate care. The symptoms can include:
- Severe headache.
- Blurry vision.
What Happens
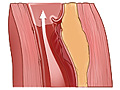
Healthy arteries have smooth inner walls. Your blood flows through them without a problem. The blood vessels stay strong and flexible.
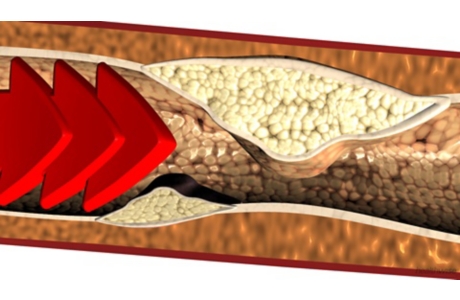
But when you have high blood pressure, blood flows through your arteries with too much force, even though you can’t feel it. Over time, this pressure damages the walls of your arteries. They aren’t smooth anymore. They get rough spots on them where fat and calcium start to build up. This buildup is called plaque (say “plak”).
Plaque is part of atherosclerosis, sometimes called “hardening of the arteries.” Over time, the plaque narrows the artery and blocks blood flow through it.
Atherosclerosis makes your arteries narrower. It also makes them stiffer. Blood can’t flow through them as easily. This lack of good blood flow starts to damage some of the organs in your body.
This damage doesn’t happen all at once. It happens slowly over time. But you can’t tell that it’s happening, because you don’t feel anything. It can lead to:
- Coronary artery disease and heart attack.
- Heart failure.
- Stroke.
- Kidney failure.
- Peripheral arterial disease.
- Eye damage (retinopathy) that can lead to vision loss and blindness.
What Increases Your Risk
Things that increase your risk (risk factors) for high blood pressure include:
- A family history of high blood pressure.
- Aging.
- Eating a lot of sodium (salt).
- Drinking more than 2 alcoholic drinks a day for men or more than 1 alcoholic drink a day for women.
- Being overweight or obese.
- Lack of exercise or physical activity.
- Race. African Americans are more likely to get high blood pressure, often have more severe high blood pressure, and are more likely to get the condition at an earlier age than others. Why they are at greater risk is not known.
Other possible risk factors include:
- Low intake of potassium, magnesium, and calcium.
- Sleep apnea and sleep-disordered breathing.
- Long-term use of pain medicines like NSAIDs—for example, naproxen (such as Aleve) or ibuprofen (such as Motrin or Advil)—or COX-2 inhibitors, such as celecoxib (Celebrex). Aspirin does not increase your risk for getting high blood pressure.
When to Call a Doctor
Call 911 anytime you think you may need emergency care. This may mean having symptoms that suggest that your blood pressure is causing a serious heart or blood vessel problem. Your blood pressure may be over 180/120.
For example, call 911 if:
- You have symptoms of a heart attack. These may include:
- Chest pain or pressure, or a strange feeling in the chest.
- Sweating.
- Shortness of breath.
- Nausea or vomiting.
- Pain, pressure, or a strange feeling in the back, neck, jaw, or upper belly or in one or both shoulders or arms.
- Lightheadedness or sudden weakness.
- A fast or irregular heartbeat.
- You have symptoms of a stroke. These may include:
- Sudden numbness, tingling, weakness, or loss of movement in your face, arm, or leg, especially on only one side of your body.
- Sudden vision changes.
- Sudden trouble speaking.
- Sudden confusion or trouble understanding simple statements.
- Sudden problems with walking or balance.
- A sudden, severe headache that is different from past headaches.
- You have severe back or belly pain.
Do not wait until your blood pressure comes down on its own. Get help right away.
Call your doctor now or seek immediate care if:
- Your blood pressure is much higher than normal (such as 180/120 or higher), but you don’t have symptoms.
- You think high blood pressure is causing symptoms, such as:
- Severe headache.
- Blurry vision.
Watch closely for changes in your health, and be sure to contact your doctor if:
- Your blood pressure measures higher than your doctor recommends at least 2 times. That means the top number is higher or the bottom number is higher, or both.
- You think you may be having side effects from your blood pressure medicine.
Who to see
Your blood pressure can be checked:
- At a clinic where you work or go to school.
- At pharmacies, health fairs, fitness centers, community centers, fire stations, and ambulance stations.
- By a nurse practitioner or physician assistant.
- By a primary care doctor.
For diagnosis and management of high blood pressure, see:
- A primary care doctor.
- An internist.
- A cardiologist (heart specialist). In general, a cardiologist is needed only in cases of extremely high blood pressure or when the person has other serious heart problems.
- A nephrologist (kidney specialist), in extreme cases.
- A nurse practitioner.
- A physician assistant.
Exams and Tests
The main test for high blood pressure is simple, fast, and painless. These are the usual steps:
- You sit quietly for 5 minutes before the test, with both feet flat on the floor.
- You sit down with your arm resting on the arm of the chair so that your arm is level with your heart.
- An inflatable sleeve, called a cuff, is wrapped around your upper arm. It’s attached to a dial that will show your blood pressure numbers.
- The nurse (or other health professional) seals the cuff and pumps it up. You feel tight pressure as the cuff cuts off the blood flow in your arm.
- Next, the nurse slowly loosens the cuff while using a stethoscope to listen to the heartbeat in your inner elbow. When the cuff is just loose enough that blood starts to flow again and the nurse can hear it, that is your systolic blood pressure.
- The cuff is slowly loosened some more. When it’s loose enough that your heartbeat can no longer be heard through the stethoscope, that is your diastolic blood pressure.
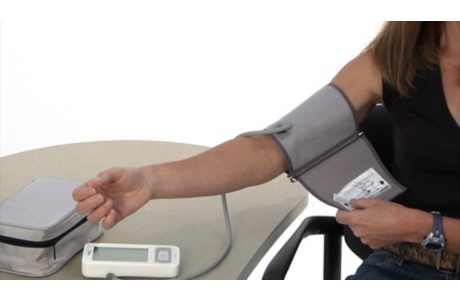
After measuring your blood pressure, your doctor may ask you to test it again when you are home.footnote 1, footnote 3 This is because your blood pressure can change throughout the day. And sometimes blood pressure is high only because you are seeing a doctor. This is called white-coat hypertension. To diagnose high blood pressure, your doctor needs to know if your blood pressure is high throughout the day.
So your doctor may ask you to monitor your blood pressure at home to make sure that it actually is high. You may get an ambulatory blood pressure monitor or a home blood pressure monitor. These devices measure your blood pressure several times throughout the day.
Regular blood pressure checks
All adults should have their blood pressure checked regularly.footnote 3
Your doctor can let you know how often you should get your blood pressure checked. It may depend on what your blood pressure is and your risk for heart disease. You can get your blood pressure checked during any routine medical visit.
The U.S. Preventive Services Task Force (USPSTF) makes these recommendations about how often to check your blood pressure:footnote 3
- Get your blood pressure checked every year if any one of the following is true:
- You’re age 40 or older.
- You’re African-American.
- You’re overweight or obese.
- The top number of your blood pressure is 130 to 139, or the bottom number is 85 to 89, or both.
- You can get your blood pressure checked every 3 to 5 years if allof the following are true:
- You’re age 18 to 39.
- Andthe top number of your blood pressure is lower than 130, and the bottom number is lower than 85.
- And you’re not African-American, overweight, or obese.
The automated devices you find in grocery stores or drugstores may not be accurate. Having your blood pressure checked at the doctor’s office is best.
A home blood pressure monitor makes it easy to keep track of your blood pressure. It’s a good idea to bring your home monitor to the doctor’s office to check its accuracy.
Other tests
Besides taking your blood pressure, your doctor will do a physical exam and medical history. Your doctor may also have you get other tests to find out whether high blood pressure has damaged any organs or caused other problems. These tests may include:
- Urine tests to check for kidney disease.
- Blood tests to check your levels of potassium, sodium, and cholesterol.
- A blood glucose test to check for diabetes.
- Tests to measure kidney function.
- An electrocardiogram (EKG, ECG) to find out whether there is any damage to the heart.
Your doctor may also check your risk of a heart attack and stroke.
If your doctor recommends a test, ask what it is for and why you need it. You can help decide if a test is right for you. Talk with your doctor to make that decision. For more information, see Heart Tests: When Do You Need Them?
Treatment Overview
Untreated high blood pressure can lead to heart attacks or strokes. The higher your blood pressure, the greater your risk. Lowering blood pressure lowers the risk of damaging blood vessels and getting atherosclerosis.
High blood pressure usually can’t be cured. But it can be controlled. The two types of treatment for high blood pressure are:
- Lifestyle changes.
- Daily medicines.
Your doctor will give you a goal for your blood pressure. This goal will be based on your health and your age. Your blood pressure goal can help you prevent problems caused by high blood pressure.
Treating high blood pressure with lifestyle changes
For some people, lifestyle changes may be enough to lower their blood pressure. Whether this is an option for you depends on how high your blood pressure is and whether you have other health problems, such as diabetes or heart disease.
Your doctor may suggest that you make one or more of the following changes:
- Lose weight. If you’re overweight, losing extra pounds may bring your blood pressure down.
- Get more active. Regular aerobic exercise can help lower blood pressure.
- Stop smoking. Smoking increases your risk for heart attack and stroke.
- Limit alcohol. Limit alcohol to 2 drinks a day for men, 1 drink a day for women.
- Eat less sodium. To help lower blood pressure, try to eat less than 1,500 mg a day.
- Follow the DASH diet. The DASH (Dietary Approaches to Stop Hypertension) eating plan can help you lower your blood pressure.
For tips on how to do these things, see the Living With High Blood Pressure section of this topic.
 One Woman’s Story: Izzy, 60 “I could never have imagined I could get (my blood pressure) down so low by losing weight. I feel sure it was the WAY I lost weight, with DASH.”— Izzy |
Treating high blood pressure with medicines
If lifestyle changes don’t lower your blood pressure to your goal, you may need to take daily medicines as well.
Medicines control—but usually don’t cure—high blood pressure. So you will probably need to take them for the rest of your life. Most people need to take two or more medicines.
Some people find it hard to take their medicines properly. They may feel it’s too much trouble—especially when they don’t feel sick. Or they’re worried about side effects. Some people find it hard to keep track of when and how to take their medicines.
If you have trouble taking high blood pressure medicines for any reason, talk to your doctor.
 One Man’s Story: Tyrell, 35 “I learned that it doesn’t matter how healthy you feel—if you have high blood pressure, you’re sick and you’d better do something about it.”— Tyrell Read more about Tyrell and why he started taking his medicines properly. |
Prevention
A heart-healthy lifestyle can help you prevent high blood pressure. These changes are especially important for people who have risk factors for high blood pressure that cannot be changed, including family history, race, or age.
Here are some things you can do:
- Stay at a healthy weight.
- Eat heart-healthy foods, and limit sodium.
- Get regular exercise.
- Limit alcohol.
For help with all of these, see the Living With High Blood Pressure section of this topic.
Living With High Blood Pressure
Heart-healthy lifestyle changes are important to help control high blood pressure. These changes can help lower your risk for coronary artery disease, heart attack, and stroke.
A heart-healthy lifestyle is always important, even if you take medicines too. Some people can even take less medicine after making these changes.
What changes do you need to make?
Make these lifestyle changes to help lower your blood pressure and lower your risk for heart attack and stroke:
- Lose extra weight. If you are overweight, losing as little as 10 lb (4.5 kg) may lower your blood pressure. It may also allow you to take less blood pressure medicine.
- Eat heart-healthy foods. Getting enough of the nutrients found in fruits, vegetables, and dairy products helps lower blood pressure. Use the DASH eating plan as a guide. See the topic High Blood Pressure: Nutrition Tips.
- Get active. Regular physical activity can lower blood pressure in those who have high blood pressure. Try to do moderate activity at least 2½ hours a week. Or try to do vigorous activity at least 1¼ hours a week.
- Drink less alcohol. Alcohol increases blood pressure. Drink it in moderation, if at all. That means no more than 2 drinks a day for men or 1 drink a day for women.
- Cut back on sodium. Eating less sodium can help prevent and control high blood pressure. Try to limit the amount of sodium you eat to less than 1,500 mg a day.
- Manage stress. Your blood pressure increases when you are under stress. Relaxation techniques, including progressive muscle relaxation and meditation, may help lower mild high blood pressure. For more information, see the topic Stress Management.
- Check your own blood pressure. A home blood pressure monitor makes it easy to keep track of your blood pressure. Seeing those small improvements can motivate you to keep going with your lifestyle changes.
Quitting smoking is also important to reduce your risk of heart attack and stroke. For more information, see the topic Quitting Smoking.
How do you make lifestyle changes?
Making any kind of change in the way you live your daily life is like being on a path. The path leads to success. Here are the first steps on that path:
- Have your own reason for making a change. If you do it because someone else wants you to, you’re less likely to have success. When you have high blood pressure, the reason for making lifestyle changes is clear: to lower your blood pressure and your risk for a heart attack and stroke. If you don’t feel ready now, learn more about high blood pressure and the damage it can do. When you truly want to make changes, you’re ready for the next step.
- Set goals. Include long-term goals as well as short-term goals that you can measure easily. Your doctor can help you figure out what your long-term goals should be for your blood pressure. Short-term goals are the small steps you take, week by week, to improve your health.
- Measure improvements to your health. Before you make lifestyle changes, ask your doctor to check your blood pressure. Then, as you start to make changes, have your blood pressure checked often, and keep track of the numbers. You can buy a home blood pressure monitor that is easy to use.
- Think about what might get in your way, and prepare for slip-ups. By thinking about these barriers now, you can plan ahead for how to deal with them if they happen. Use a personal action plan( What is a PDF document? ) to write down your barriers and backup plans.
- Get support from your family, your doctor, and your friends. Tell them about your long-term and short-term goals and how they can help.
For help making lifestyle changes, see the topic Change a Habit by Setting Goals.
 One Woman’s Story: Izzy, 60 “A big lesson I learned is that everything we do routinely is a habit. And habits can be changed. I’m living proof.”— Izzy |
 One Man’s Story: Arturo, 58 “As soon as I mentioned [to my wife] that I needed help, she got out a pen and some paper and started writing out a walking schedule.”— Arturo Read more about Arturo and how he got support for his lifestyle changes. |
Medications
Deciding whether to treat high blood pressure with medicine and choosing the best medicine may depend on:
- How high your blood pressure is and what your blood pressure goal is.
- Whether you have signs that high blood pressure has caused organ damage, such as an enlarged heart or early damage to your arteries, kidneys, or eyes.
- Whether you have other medical conditions, such as coronary artery disease, diabetes, or kidney or lung disease or risk factors for heart disease, such as diabetes or high cholesterol.
- Whether you think you can succeed at making lifestyle changes.
Doctors usually prescribe a single, low-dose medicine first. If blood pressure is not controlled, your doctor may change the dosage or try a different medicine or combination of medicines. It is common to try several medicines before blood pressure is successfully controlled. Many people need more than one medicine to get the best results.
Medicine choices
Medicine choices include:
- Diuretics.
- ACE inhibitors.
- Angiotensin II receptor blockers (ARBs).
- Beta-blockers.
- Calcium channel blockers.
- Direct renin inhibitors.
- Other medicines for high blood pressure, including alpha-blockers and vasodilators.
All of these medicines are effective for lowering the risk of heart attack and stroke.
Work with your doctor to find the right medicine or combination of medicines that have the fewest side effects and work well for you. And be sure to take your medicines regularly as prescribed.
You may have regular blood tests to monitor how the medicine is working in your body. Your doctor will likely let you know when you need to have the tests.
 One Man’s Story: Tyrell, 35 “For a few months I was really good about taking (my pills) every day. But they made me a little tired, and I got tired of being tired.”— Tyrell Read more about Tyrell and why he returned to taking his medicine every day. |
What to think about
- The medicine your doctor chooses may be based on other health problems you have. For example, doctors often prescribe ACE inhibitors for people who have diabetes or heart failure.
- Some people who get a cough while taking ACE inhibitors do well with ARBs, which usually don’t cause a cough.
- You may need to avoid some over-the-counter medicines. For example, check with your doctor before you take any nonsteroidal anti-inflammatory drugs (NSAIDs)—such as naproxen and ibuprofen—with high blood pressure medicines. NSAIDs may raise blood pressure and keep your blood pressure medicines from working well. NSAIDs may also interact with your blood pressure medicine and cause kidney problems.
- Don’t take any other prescription medicines, over-the-counter medicines, vitamins, or supplements unless you talk to your doctor first. Medicines can interact with each other and keep blood pressure medicines from working right or cause a bad reaction.
Other Treatment
Complementary medicine
Complementary medicine is treatment that you use in addition to your doctor’s standard care. Tell your doctor if you are using, or if you plan to use, complementary medicine to help lower your blood pressure. These treatments do not replace lifestyle changes or medicine for high blood pressure. You and your doctor can decide which therapy might be best for you.
Complementary treatments that help manage stress and improve quality of life may help lower blood pressure. These treatments include:
Most mind and body practices—such as acupuncture, meditation, and yoga—are safe when used under the care of a well-trained professional. Choose an instructor or practitioner as carefully as you would choose a doctor.
Other treatment to reduce risk of heart disease
There are some dietary supplements that you may hear about to lower the risk of heart disease, heart attack, and stroke. It is not clear if some vitamins, minerals, and multivitamins can lower risk. But it is clear that some supplements, such as vitamin E and beta-carotene, do not lower risk.footnote 4
Talk with your doctor about the best ways to lower your risk of heart disease, heart attack, and stroke. Tell your doctor if you plan to use dietary supplements or vitamins. Your doctor can make sure they are safe for you.
References
Citations
- Whelton PK, et al. (2017). Guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Journal of the American College of Cardiology, published online November 13, 2017. DOI: 10.1016/j.jacc.2017.11.006. Accessed November 20, 2017.
- Benjamin EJ, et al. (2017). Heart disease and stroke statistics—2017 update: A report from the American Heart Association. Circulation, 135(10): e146–e603. DOI: 10.1161/CIR.0000000000000485. Accessed January 26, 2017.
- U.S. Preventive Services Task Force (2015). Hypertension in adults: Screening and home monitoring: Final recommendation statement. http://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/high-blood-pressure-in-adults-screening. Accessed January 21 , 2016.
- U.S. Preventive Services Task Force (2014). Vitamin, mineral, and multivitamin supplements for the primary prevention of cardiovascular disease and cancer. U.S. Preventive Services Task Force. http://www.uspreventiveservicestaskforce.org/uspstf/uspsvita.htm. Accessed March 28, 2014.
Other Works Consulted
- Aronow WS, et al. (2011). ACCF/AHA 2011 Expert consensus document on hypertension in the elderly: A report of the American College of Cardiology Foundation Task Force on Clinical Expert Consensus Documents. Circulation, 123(21): 2434–2506.
- Atkins GB, et al. (2011). Diagnosis and treatment of hypertension. In V Fuster et al., eds., Hurst’s the Heart, 13th ed., vol. 2, pp. 1585–1605. New York: McGraw-Hill.
- Brook RD, et al. (2013). Beyond medications and diet: Alternative approaches to lowering blood pressure. A scientific statement from the American Heart Association. Hypertension, 61(6): 1360–1383. DOI: 10.1161/HYP.0b013e318293645f. Accessed February 19, 2014.
- Cheriyan J, et al. (2010). Primary prevention of CVD: treating hypertension, search date December 2007. Online version of BMJ Clinical Evidence: http://www.clinicalevidence.com.
- Eckel RH, et al. (2013). 2013 AHA/ACC guideline on lifestyle management to reduce cardiovascular risk: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. http://circ.ahajournals.org/content/early/2013/11/11/01.cir.0000437740.48606.d1.citation. Accessed December 5, 2013.
- Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents (2011). Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: Summary report. Pediatrics, 128(Suppl 5): S213–S256.
- Go AS, et al. (2013). An effective approach to high blood pressure control: A scientific advisory from the American Heart Association, the American College of Cardiology, and the Centers for Disease Control and Prevention. Hypertension. DOI: 10.1161/HYP.0000000000000003. Accessed December 30, 2013.
- Henri HC, Rudd P (2007). Hypertension: Context and management. In EJ Topol, ed., Textbook of Cardiovascular Medicine, 3rd ed., pp. 88–108. Philadelphia: Lippincott Williams and Wilkins.
- James PA, et al. (2013). 2014 Evidence-based guideline for the management of high blood pressure in adults: Report from the panel members appointed to the Eighth Joint National Committee (JNC 8). Journal of the American Medical Association. DOI: 10.1001/jama.2013.284427. Accessed December 18, 2013.
- National Heart, Lung, and Blood Institute (2006). Your Guide to Lowering Your Blood Pressure With DASH (NIH Publication No. 06-4082). Available online: http://www.nhlbi.nih.gov/health/public/heart/hbp/dash/new_dash.pdf.
- Pickering TG, et al. (2008). Call to action on use and reimbursement for home blood pressure monitoring. A joint scientific statement from the American Heart Association, American Society of Hypertension, and Preventive Cardiovascular Nurses Association. Hypertension, 52(1): 10–29.
- U.S. Department of Health and Human Services (2008). 2008 Physical Activity Guidelines for Americans (ODPHP Publication No. U0036). Washington, DC: U.S. Government Printing Office. Available online: http://www.health.gov/paguidelines/guidelines/default.aspx.
- U.S. Preventive Services Task Force. (2015). Hypertension in Adults: Screening and Home Monitoring: Final Recommendation Statement. http://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/high-blood-pressure-in-adults-screening. Accessed January 21 , 2016
- Weber MA, et al. (2013). Clinical practice guidelines for the management of hypertension in the community. Journal of Clinical Hypertension. DOI: 10.1111/jch.12237. Accessed December 19, 2013.
Current as of: April 9, 2019
Author: Healthwise Staff
Medical Review:Adam Husney MD – Family Medicine & Kathleen Romito MD – Family Medicine & E. Gregory Thompson MD – Internal Medicine & Martin J. Gabica MD – Family Medicine
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.